The Power of Non-Medical Influences in Modern Healthcare
In today’s evolving healthcare ecosystem, the Social Determinants of Health (SDOH) have become the cornerstone of equitable, preventive, and patient-centered care. These non-medical factors—ranging from housing and education to food access and social support—determine how well individuals can maintain their health, manage chronic diseases, and recover from illness. While clinical care remains critical, research consistently shows that nearly 80% of health outcomes depend on SDOH rather than medical treatment alone. Understanding and addressing these determinants allow healthcare providers, policymakers, and community organizations to craft holistic care models that improve lives beyond the clinic walls.
Understanding the Concept of SDOH
The World Health Organization defines Social Determinants of Health as “the conditions in which people are born, grow, live, work, and age.” These factors influence daily choices, access to healthcare, and even life expectancy. In simpler terms, a person’s zip code often predicts health outcomes more accurately than their genetic code.
Healthcare organizations have categorized SDOH into five major domains:
- Economic Stability – Employment, income, and financial resilience directly impact a patient’s ability to afford care, food, or medication.
- Education Access & Quality – Literacy, language proficiency, and educational attainment determine how well patients understand health information.
- Healthcare Access & Quality – This includes insurance coverage, provider availability, and cultural or language barriers.
- Neighborhood & Built Environment – Housing safety, pollution levels, food deserts, and local crime rates shape overall well-being.
- Social & Community Context – Family support, discrimination, and social networks influence emotional stability and community engagement.
These domains form the framework that healthcare organizations use to identify and address non-clinical risk factors.
The Clinical Impact of SDOH
Clinicians are witnessing firsthand that SDOH are not abstract concepts—they affect real-world outcomes. Patients with unstable housing may lack refrigeration for insulin; those in food-insecure areas struggle to maintain balanced diets; and individuals without reliable transportation frequently miss follow-up appointments.
Common SDOH Challenges in Healthcare Settings:
- Missed or delayed care appointments due to transport barriers.
- Poor medication adherence caused by financial stress.
- Increased emergency department (ED) visits due to unmanaged chronic conditions.
- Fragmented communication between medical and community care teams.
By systematically identifying these risks, providers can prevent avoidable hospitalizations and improve care continuity.
Screening and Identifying SDOH in Clinical Workflows
To make SDOH actionable, healthcare teams have integrated standardized screening tools into patient workflows. Among the most popular tools are:
- PRAPARE (Protocol for Responding to and Assessing Patients’ Assets, Risks, and Experiences): Widely used by Federally Qualified Health Centers (FQHCs) to collect social risk data.
- AHC-HRSN (Accountable Health Communities Health-Related Social Needs): Developed by CMS for consistent use in Medicare and Medicaid programs.
- State Medicaid SDOH Forms: These tailor screenings to regional health priorities and funding models.
Screenings often occur during annual wellness visits, intake appointments, or post-hospital discharge calls. Once social risks are identified, care teams can initiate referrals to community resources—like food banks, housing agencies, or transportation programs—ensuring that patients receive comprehensive support.
The Technology Behind SDOH Data Management
Collecting SDOH data is only one part of the puzzle. Managing and sharing it securely is another. Clinics now use technology frameworks like FHIR (Fast Healthcare Interoperability Resources) and ICD-10 Z-codes to record, exchange, and analyze SDOH data while maintaining HIPAA compliance.
Key Benefits of Digital SDOH Systems:
- Structured Data Entry: EHR-integrated templates streamline documentation.
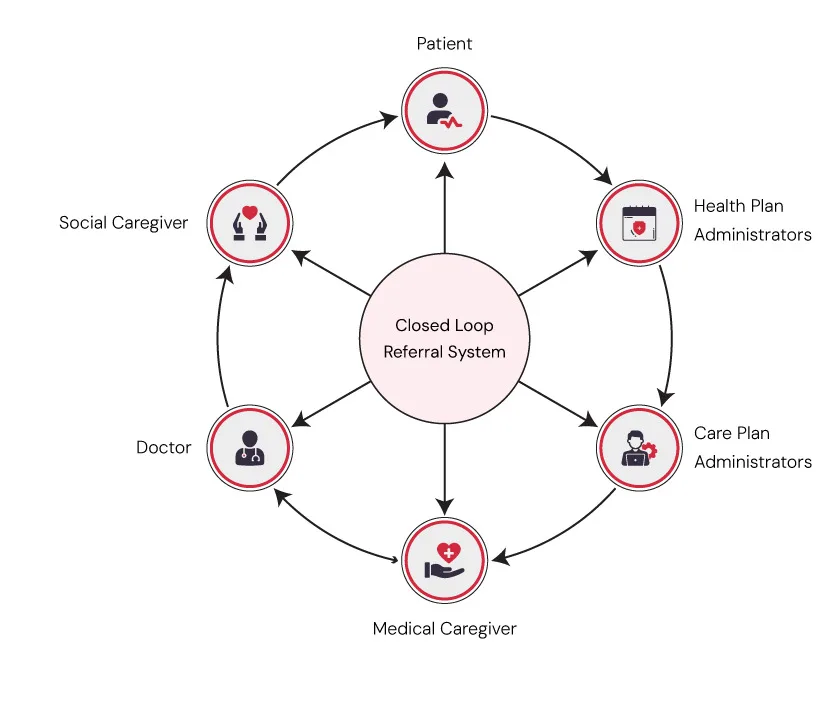
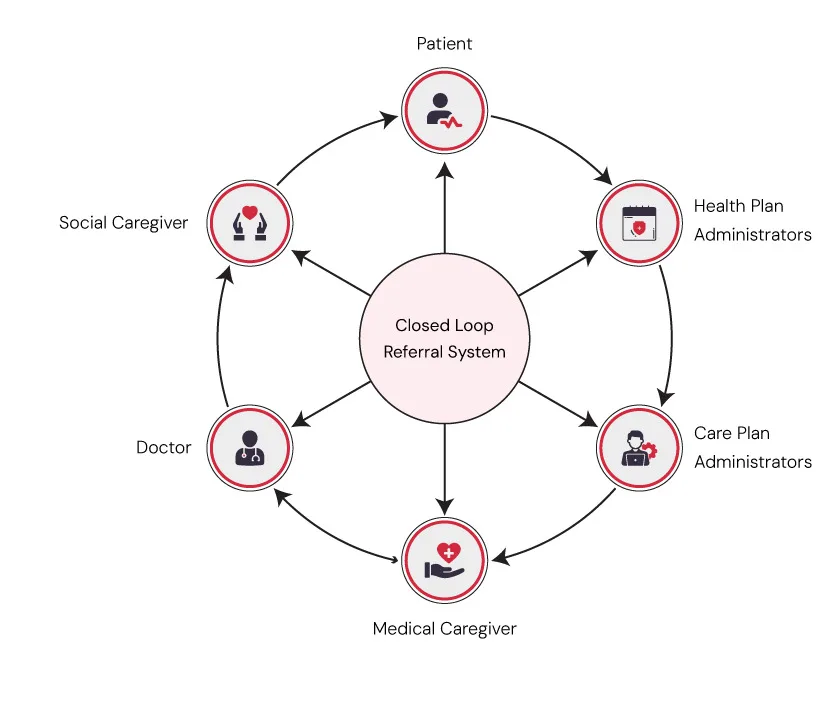
- Closed-Loop Referrals: Automated updates show whether patients received help.
- Team Collaboration: Care managers and community partners can coordinate efficiently.
- Analytics for Value-Based Care: Data-driven insights improve reporting and quality metrics.
For example, platforms like Pillar Healthcare Software by SocialRoots.ai simplify this process with automated referrals, digital screenings, and real-time dashboards—enabling care teams to manage high-risk populations effectively.
Turning Data Into Action: Real Interventions That Work
Healthcare organizations can’t stop at data collection—they must translate insights into interventions. Successful SDOH programs often include:
- Food Security Programs: Partnering with community food pantries to improve chronic disease management.
- Transportation Assistance: Providing rides to medical appointments reduces no-show rates.
- Housing Stability Initiatives: Collaborating with local agencies to secure safe living environments.
- Behavioral and Social Support: Connecting patients with social workers or mental health professionals.
- Community Resource Navigation: Helping patients identify and access local support systems.
When these interventions are coordinated, patients experience fewer emergency visits, improved adherence to care plans, and greater overall satisfaction.
Operational Challenges in Addressing SDOH
Despite the progress, implementing SDOH strategies at scale is not without barriers. Clinics often face:
- Data Silos: SDOH information trapped within electronic health records, inaccessible to community partners.
- Manual Tracking: Care teams rely on spreadsheets or phone calls, limiting efficiency.
- Referral Drop-offs: Lack of communication prevents feedback on completed services.
- Staff Fatigue: Overworked clinicians may deprioritize SDOH screening.
The solution lies in digital transformation—automating processes, integrating community networks, and leveraging data to close care gaps.
The Future of Healthcare: SDOH as a Core Strategy
As healthcare shifts toward value-based care, SDOH integration is no longer optional—it’s essential. Health systems that embed social determinants into their workflows gain measurable advantages:
- Better population health outcomes.
- Improved patient trust and engagement.
- Higher reimbursement through quality-based metrics.
- Reduced healthcare costs from preventable admissions.
By prioritizing SDOH, organizations move beyond reactive care and embrace proactive, human-centered health management.
Building Partnerships for Sustainable Change
No single entity can solve the challenges of SDOH alone. Collaborative networks between hospitals, local governments, nonprofits, and tech providers form the foundation of sustainable progress.
These partnerships ensure that care extends beyond clinical walls—creating a safety net where medical care and social support intersect seamlessly.
For instance, integrating digital systems like Pillar by SocialRoots.ai allows for automatic referrals to social services, ensuring patients never fall through the cracks. Such innovations are setting new standards for equity-driven healthcare.
Conclusion: Redefining Care Through SDOH
Health is more than prescriptions and procedures—it’s shaped by the environments people live in and the resources they can access. When healthcare systems address Social Determinants of Health (SDOH), they empower patients to take control of their well-being and close the gap between clinical care and everyday life.
To truly understand What Is SDOH, organizations must view it not as an add-on but as the foundation of equitable healthcare. By transforming data into action, technology into compassion, and partnerships into prevention, we can build a healthier, fairer future for all.