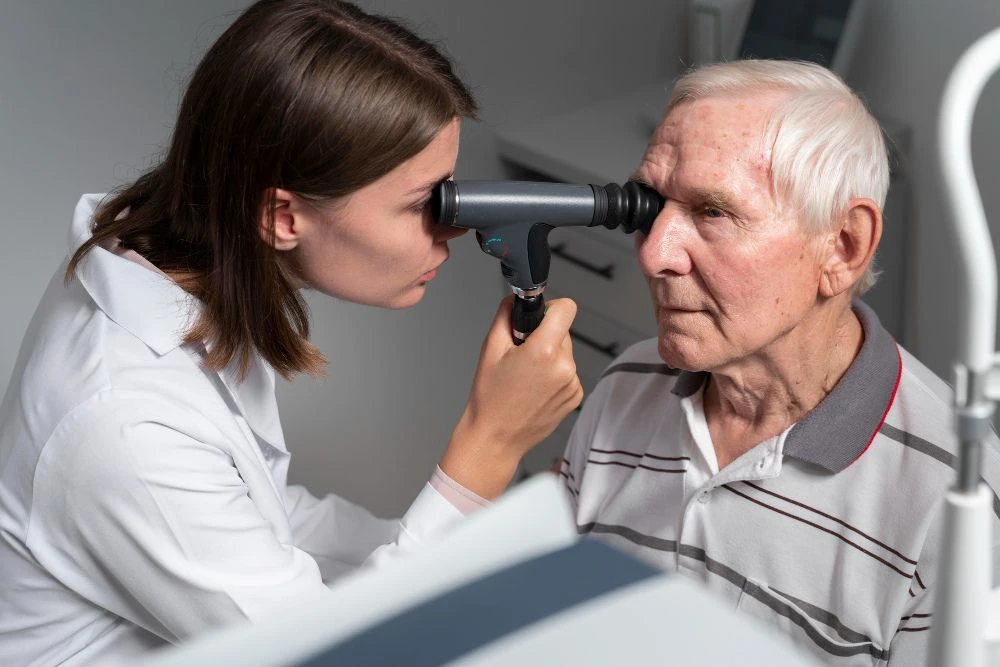
Diabetes is one of the leading causes of blindness in working-age adults worldwide. Among its many complications, diabetic retinopathy (DR) stands out as the most common and most feared. This sight-threatening condition develops silently over years, often without early symptoms, until irreversible damage has already occurred. Fortunately, vision loss from diabetic retinopathy is largely preventable when the disease is detected and treated early by a qualified diabetic retinopathy specialist.
A diabetic retinopathy specialist is typically a retina-trained ophthalmologist (vitreoretinal surgeon or medical retina specialist) with advanced fellowship training in the diagnosis, monitoring, and treatment of retinal vascular diseases, including diabetic retinopathy and diabetic macular edema (DME). Their expertise goes far beyond routine eye exams performed by general ophthalmologists or optometrists. These specialists possess the clinical experience, diagnostic tools, and therapeutic options required to halt progression and, in many cases, reverse vision-threatening changes before permanent blindness occurs.
Understanding Diabetic Retinopathy: The Silent Threat
Diabetic retinopathy occurs when prolonged high blood glucose damages the tiny blood vessels that nourish the retina — the light-sensitive tissue at the back of the eye. In the early stage, known as non-proliferative diabetic retinopathy (NPDR), blood vessels weaken, leak fluid, or form microaneurysms. Many patients remain completely asymptomatic during this phase.
As the disease advances to proliferative diabetic retinopathy (PDR), the retina grows fragile new blood vessels in an attempt to supply oxygen. These abnormal vessels are prone to bleeding (vitreous hemorrhage) and can cause severe scar tissue formation, leading to tractional retinal detachment — one of the most devastating complications.
Diabetic macular edema (DME), which can occur at any stage, happens when fluid leaks into the central retina (macula), causing swelling and blurred central vision required for reading, driving, and recognizing faces. DME is now the leading cause of vision loss in diabetic patients.
Without intervention from a diabetic retinopathy specialist, up to 50% of patients with proliferative disease can become legally blind within five years.
Why a Diabetic Retinopathy Specialist Matters More Than Ever
While primary care physicians, endocrinologists, and general eye doctors play essential roles in diabetes management, they cannot replace the targeted expertise of a diabetic retinopathy specialist. Here’s why:
- Advanced Diagnostic Precision
- Diabetic retinopathy specialists use cutting-edge imaging that goes far beyond a simple dilated eye exam:
- Wide-field and ultra-widefield fluorescein angiography to map every peripheral ischemic area
- Optical coherence tomography (OCT) and OCT-angiography (OCT-A) for micron-level detection of macular edema and neovascularization
- Fundus autofluorescence and adaptive optics to identify earliest cellular changes
- These tools allow the specialist to detect clinically significant changes months or even years before they would be visible on standard examination.
- Risk Stratification and Personalized Screening Schedules
- Not every diabetic patient progresses at the same rate. A diabetic retinopathy specialist analyzes dozens of risk factors — duration of diabetes, HbA1c trajectory, blood pressure trends, kidney function, pregnancy status, sleep apnea, and even genetic markers — to create an individualized screening and follow-up plan. Some patients may need evaluation every 3–4 months, while well-controlled individuals can safely extend to 12–24 months.
- State-of-the-Art Treatment Options
- When intervention is required, diabetic retinopathy specialists offer the full spectrum of evidence-based therapies:
- Anti-VEGF Injections (Lucentis, Eylea, Vabysmo, faricimab)
- Today’s cornerstone treatment for diabetic macular edema and proliferative retinopathy. Multiple landmark clinical trials (Protocol T, PANORAMA, YOSEMITE/RHINE) have shown that regular anti-VEGF therapy can improve vision in over 50–70% of patients with DME and dramatically reduce the risk of severe vision loss in PDR.
- Longer-acting agents and port-delivery systems (Susvimo) and gene therapy approaches currently in trials are expanding treatment durability and reducing injection burden — options only a diabetic retinopathy specialist can appropriately select and administer.
- Laser Photocoagulation
- Though less commonly used as first-line therapy today, targeted navigated laser (PASCAL, Navilas) and pattern-scanning laser still play important roles in select cases of severe NPDR, persistent DME, and peripheral ischemia.
- Vitrectomy Surgery
- For advanced complications such as non-clearing vitreous hemorrhage, tractional retinal detachment, or ghost-cell glaucoma, diabetic retinopathy specialists perform minimally invasive 27-gauge vitrectomy with better outcomes and faster recovery than ever before.
- Intravitreal Steroids and Implants
- For patients who respond poorly to anti-VEGF or cannot tolerate frequent injections, long-acting steroid implants (Ozurdex, Iluvien, Yutiq) provide alternative pathways managed exclusively by retina specialists.
- Coordination of Systemic Control
- The best diabetic retinopathy specialist never works in isolation. They communicate directly with endocrinologists when rapid tightening of glucose control paradoxically worsens retinopathy (early worsening phenomenon), advise nephrologists about contrast dye safety in angiography when kidney function is impaired, and guide obstetricians in high-risk diabetic pregnancies where retinopathy can accelerate dramatically.
The Proven Impact on Vision Preservation
Large population studies consistently demonstrate the dramatic difference a diabetic retinopathy specialist makes:
- The Diabetic Retinopathy Clinical Research Network (DRCR.net) showed that patients followed by retina specialists had a 50–70% lower risk of severe vision loss compared to standard care.
- In the United Kingdom, the introduction of systematic screening combined with prompt referral to diabetic retinopathy specialists reduced diabetes-related blindness by over 50% in a decade.
- Real-world data from the American Academy of Ophthalmology IRIS Registry (2014–2020) revealed that patients treated with anti-VEGF under retina specialist care gained an average of 8–12 letters of vision, whereas untreated or delayed-treatment cohorts lost vision progressively.
When Should You See a Diabetic Retinopathy Specialist?
Referral to a diabetic retinopathy specialist is recommended in the following situations:
- Any level of diabetic macular edema
- Moderate non-proliferative DR or worse (ETDRS level 43 or higher)
- Proliferative diabetic retinopathy (new vessels, pre-retinal hemorrhage)
- Unexplained vision loss in a diabetic patient
- High-risk features on OCT or wide-field imaging (extensive ischemia, subclinical neovascularization)
- Pregnancy in a patient with pre-existing diabetes (ideally pre-conception evaluation)
- Before bariatric surgery or initiation of insulin pump/SGLT2/GLP-1 therapy when rapid glycemic improvement is anticipated
Even patients with mild NPDR benefit from at least one baseline evaluation by a diabetic retinopathy specialist to establish risk profile and imaging baseline.
The Future: AI, Home Monitoring, and Beyond
Diabetic retinopathy specialists are embracing artificial intelligence and telemedicine to extend their reach. FDA-approved autonomous AI systems (IDx-DR, EyeArt) now accurately detect more-than-mild DR in primary care settings, enabling faster triage to specialists. Home OCT devices and smartphone-based fundus photography are entering clinical trials, potentially allowing high-risk patients to transmit images directly to their diabetic retinopathy specialist between visits.
Emerging therapies such as oral medications targeting the renin-angiotensin system, neuroprotective agents, and gene therapies silencing VEGF production are all in late-stage trials. Retina specialists remain at the forefront of enrolling patients in these groundbreaking studies.
Taking Control of Your Vision
The message is clear: diabetic retinopathy is not an inevitable consequence of diabetes, and blindness is no longer an acceptable outcome. With early detection and expert management, over 90% of vision loss can be prevented.
If you or a loved one has diabetes — particularly if it has been present for more than 10 years, blood sugar control has been challenging, or any blurring or dark spots have appeared — do not wait for symptoms to worsen. Ask your doctor for a referral to a diabetic retinopathy specialist today.
Your vision is irreplaceable, but with the right specialist on your team, it is also highly protectable.