A septal perforation is a medical condition characterized by a hole or defect in the nasal septum, the wall that separates the two nostrils. This condition can cause discomfort, frequent nosebleeds, nasal congestion, and sometimes whistling sounds during breathing. Selecting the right approach for septal perforation treatment is essential to restore normal nasal function and prevent further complications. Depending on the size of the perforation, the underlying cause, and patient-specific factors, treatment can be either non-surgical or surgical. Understanding these options can help patients make informed decisions in consultation with their ENT specialists.
Understanding Septal Perforations
The nasal septum is composed of cartilage and bone, and it plays a crucial role in supporting the nose and regulating airflow. A perforation in this structure can arise due to several causes, including trauma, previous nasal surgery, prolonged use of nasal sprays, infections, or chronic inflammation. In rare cases, systemic diseases like granulomatosis with polyangiitis or certain autoimmune conditions may contribute to septal perforations.
Small perforations may not always cause symptoms, but larger or symptomatic defects often interfere with normal breathing, lead to crusting inside the nose, and increase the risk of recurrent infections. The severity of symptoms often determines the urgency and type of treatment.
Non-Surgical Methods
Non-surgical interventions are typically considered for small to medium perforations or for patients who are not ideal candidates for surgery due to health risks or personal preference. These approaches focus primarily on symptom management and maintaining nasal comfort.
Nasal Moisturizers and Saline Sprays
Regular application of nasal saline sprays or gels can help keep the nasal lining moist, reducing crusting and irritation. Moisturizing the nasal passages is especially important for patients with dry nasal mucosa, which can exacerbate discomfort.
Septal Buttons
A septal button is a medical device designed to temporarily close the perforation. Made from silicone or biocompatible materials, these buttons act as a barrier, preventing airflow through the hole and reducing whistling or bleeding. While not a permanent solution, septal buttons can significantly improve the quality of life for patients who cannot undergo surgery.
Avoiding Irritants
Lifestyle adjustments are also part of non-surgical care. Patients are advised to avoid nasal irritants such as smoke, strong chemicals, and excessive use of nasal sprays that contain steroids or decongestants. These measures can help prevent the perforation from enlarging and reduce inflammation in the surrounding tissue.
Surgical Treatment Options
Surgery is the definitive treatment for septal perforations, especially for larger defects or cases where non-surgical methods fail to provide relief. Surgical approaches aim to close the perforation permanently and restore normal nasal structure and function.
Local Flap Surgery
Local flap surgery involves repositioning tissue from adjacent areas of the nasal septum to cover the perforation. This technique is effective for small to moderate perforations and relies on the body’s own tissue to promote healing. Surgeons may use mucoperichondrial or mucoperiosteal flaps, depending on the location and size of the defect.
Autologous Tissue Grafting
For larger perforations, surgeons may use autologous tissue grafts, often harvested from the nasal septum, ear, or even the fascia from other parts of the body. The graft is placed to bridge the defect, allowing the surrounding tissue to heal over time. This approach has high success rates but requires careful planning and precision.
Endoscopic Septal Perforation Repair
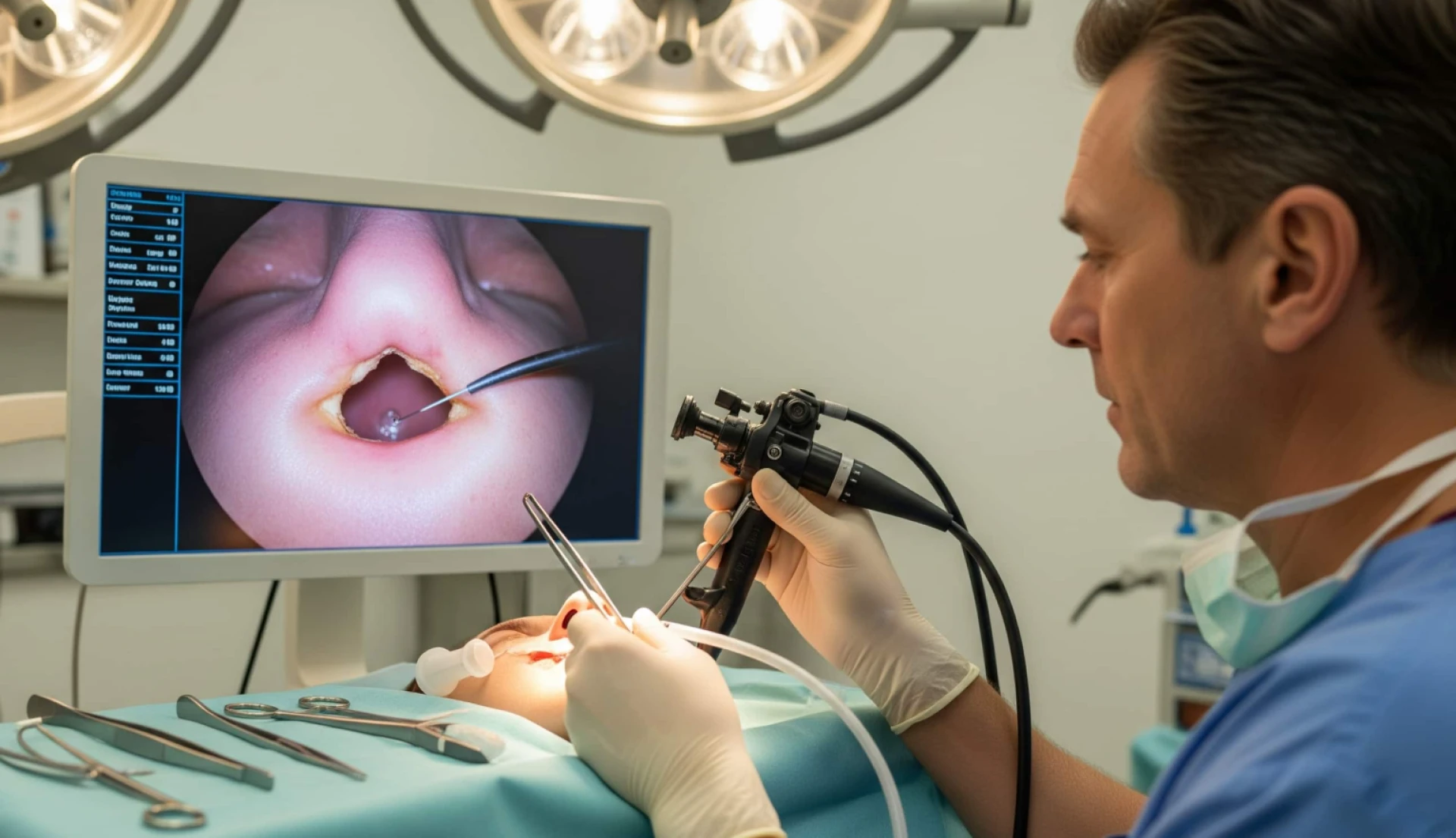
Endoscopic techniques have revolutionized septal perforation surgery by allowing minimally invasive access to the defect. Using an endoscope, surgeons can visualize the perforation and perform precise tissue manipulation. Endoscopic repair often results in reduced postoperative discomfort, faster recovery, and minimal scarring compared to traditional open approaches.
Considerations and Risks
Like any surgical procedure, septal perforation repair carries potential risks, including infection, bleeding, and recurrence of the perforation. Success depends on multiple factors, such as the size of the perforation, the quality of surrounding tissue, and patient compliance with postoperative care instructions. Surgeons typically provide detailed guidance on nasal hygiene, activity restrictions, and follow-up visits to ensure optimal outcomes.
Choosing the Right Treatment
The decision between non-surgical and surgical approaches depends on individual circumstances. Non-surgical methods are suitable for those with mild symptoms or those seeking temporary relief, while surgery offers a long-term solution for symptomatic or larger perforations. Patients should consult an experienced ENT specialist to evaluate the size, location, and cause of the perforation, as well as their overall health, before deciding on the appropriate treatment.
Factors influencing the choice of treatment include the patient’s age, general health, history of nasal surgery, and personal preferences. In many cases, a combination of therapies is employed—for instance, using a septal button initially while planning for a surgical repair at a later stage.
Recovery and Post-Treatment Care
Post-treatment care is crucial to ensure successful outcomes, whether non-surgical or surgical. For patients using septal buttons, regular cleaning and monitoring are essential to prevent infection and maintain comfort. Surgical patients require more intensive care, including nasal irrigation, avoiding strenuous activity, and attending follow-up appointments to monitor healing.
Maintaining a clean, moist nasal environment promotes tissue healing and reduces the risk of complications. Patients may also be advised to adjust their diet, hydration habits, and environmental conditions to support recovery.
Long-Term Outlook
With proper management, most patients experience significant improvement in symptoms and overall nasal function. Non-surgical approaches can offer satisfactory symptom relief for many years, while surgical repair can provide a permanent solution for eligible candidates. Regular follow-up is recommended to monitor the nasal septum and detect any recurrence or new issues promptly.
Successful septal perforation treatment not only improves breathing and comfort but also enhances overall quality of life. Patients can return to normal activities, including sports and physical exercise, without the limitations imposed by nasal discomfort or obstruction.
Conclusion
Understanding the differences between surgical and non-surgical options is key for effective septal perforation treatment. Non-surgical methods, such as septal buttons, nasal moisturizers, and lifestyle adjustments, focus on managing symptoms and providing temporary relief. Surgical options, including local flap surgery, autologous tissue grafting, and endoscopic techniques, aim to restore nasal structure and function permanently. By evaluating the size of the perforation, underlying causes, and patient-specific factors, ENT specialists can recommend the most suitable approach. Timely intervention and adherence to post-treatment care significantly improve outcomes, ensuring that patients regain normal nasal function and comfort. For those seeking long-term solutions, consulting a qualified surgeon is essential for successful septal perforation repair.