A healthy smile relies not only on the placement of advanced dental implants but also on the surrounding oral environment. Subperiosteal dental implants offer an excellent solution for patients with insufficient jawbone, providing support for missing teeth without the need for extensive bone grafting. However, one critical factor that can influence the long-term success of these implants is inflammation. Uncontrolled inflammation around the implant site can compromise tissue health, hinder healing, and even threaten the stability of the implant framework. Understanding the causes, effects, and management strategies for inflammation is essential for achieving optimal outcomes.
Understanding Subperiosteal Implants
Subperiosteal implants are uniquely designed for patients with reduced bone volume. Unlike traditional endosseous implants that are inserted directly into the jawbone, subperiosteal implants rest on top of the bone, beneath the gum tissue. This design allows patients who might otherwise require bone grafting to restore their smiles efficiently.While these implants provide a practical solution, their integration heavily relies on the health of the soft tissue surrounding the implant. Even minor inflammation can escalate, leading to complications that affect both the function and appearance of the implant.
What is Inflammation and Why It Matters
Inflammation is the body’s natural response to infection, irritation, or injury. In the context of dental implants, inflammation occurs when the soft tissues around the implant become irritated, swollen, or infected. While mild inflammation can sometimes resolve naturally, chronic or severe inflammation can hinder the healing process and compromise the stability of the implant. Key consequences of inflammation around subperiosteal implants include:
- Delayed tissue healing
- Increased risk of peri-implantitis
- Gum irritation and tenderness
- Potential loosening or failure of the implant
Understanding and controlling inflammation is therefore crucial for both immediate healing and long-term success.
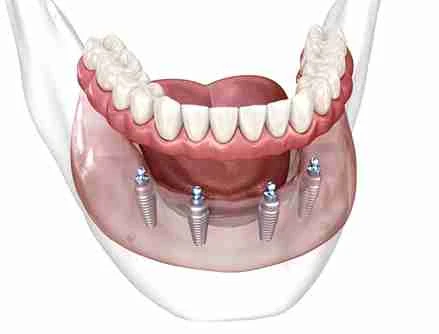
Common Causes of Inflammation Around Implants
Several factors can contribute to inflammation in patients with subperiosteal implants:
- Poor Oral Hygiene: Accumulation of plaque and bacteria around the implant framework can provoke infection and tissue irritation.
- Gum Disease: Pre-existing conditions like periodontitis or gingivitis increase susceptibility to inflammation.
- Improper Implant Placement: Incorrect positioning or excessive pressure on soft tissues can trigger an inflammatory response.
- Lifestyle Factors: Smoking, excessive alcohol, and poor dietary habits can reduce tissue healing capacity.
- Medical Conditions: Diabetes, autoimmune disorders, and other systemic conditions can impair the body’s ability to fight inflammation.
Comparison Table: Causes and Effects
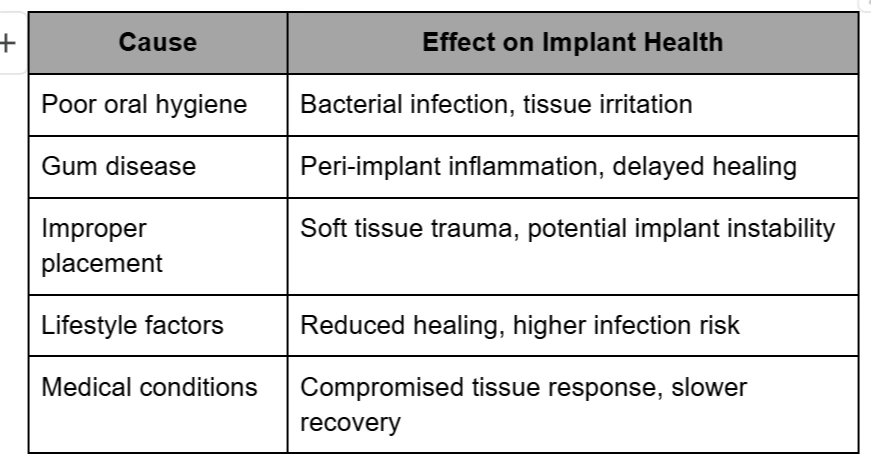
Recognising Signs of Inflammation
Early detection of inflammation around subperiosteal implants is key to preventing serious complications. Patients should look out for:
- Red, swollen, or tender gums near the implant site
- Bleeding during brushing or flossing
- Discomfort or pain around the implant
- Bad breath or pus formation
- Visible changes in gum tissue or implant positioning
Promptly addressing these symptoms with a dental professional can prevent implant failure and support long-term success.
Impact of Inflammation on Subperiosteal Implant Success
Inflammation can affect subperiosteal implants in multiple ways:
- Soft Tissue Complications: Persistent inflammation can damage gum tissue, slowing healing and increasing discomfort.
- Peri-Implantitis: Chronic inflammation may lead to bone loss around the implant, risking stability.
- Long-Term Stability Issues: Continuous tissue irritation can compromise the integration of the implant framework, potentially leading to failure.
Patients who have undergone subperiosteal dental implants Manchester or other advanced restorative procedures must pay particular attention to inflammation management, as it can directly influence both aesthetic and functional outcomes.
Preventing and Managing Inflammation
Prevention and early intervention are vital for protecting subperiosteal implants. Effective strategies include:
Lifestyle and Home Care:
- Maintain excellent oral hygiene, brushing twice daily and flossing carefully around implant sites.
- Avoid smoking and limit alcohol consumption.
- Eat a balanced diet rich in vitamins and minerals to support tissue health.
- Stay hydrated to aid in healing and oral defence.
Professional Interventions:
- Regular dental check-ups, ideally every six months, to monitor tissue health.
- Professional cleaning to remove plaque and tartar build-up around implants.
- Prescription antimicrobial rinses or treatments to combat infection.
- Digital imaging and tissue assessment to identify early signs of inflammation.
Treatment Approaches for Active Inflammation:
- Antibiotics or antimicrobial therapies for bacterial infections
- Soft tissue management and debridement for gum irritation
- Surgical intervention in severe cases of peri-implantitis
Proactive care ensures that inflammation is kept under control, allowing implants to heal effectively and remain functional long-term.
The Role of Bite Alignment in Subperiosteal Implant Longevity
Proper bite alignment is a crucial yet often overlooked factor in ensuring the long-term success of subperiosteal dental implants. Misaligned teeth or uneven occlusion can place excessive stress on the implant framework and surrounding soft tissues, increasing the risk of inflammation, discomfort, and even implant failure.
Key Considerations:
- Occlusal Balance: Ensures force is evenly distributed across all teeth and implants.
- Regular Adjustments: Minor corrections may be needed after implant placement to maintain alignment.
- Protective Measures: Custom night guards can reduce damage caused by bruxism or clenching.
By maintaining optimal bite alignment, patients safeguard their implants while improving chewing efficiency and overall oral comfort. This proactive approach complements oral hygiene, tissue care, and professional monitoring to enhance implant stability.
Long-Term Monitoring for Success
Even after successful implant placement, ongoing monitoring is essential:
- Attend scheduled dental appointments for soft tissue evaluation and implant stability checks.
- Maintain optimal oral hygiene practices consistently.
- Report any discomfort, bleeding, or unusual changes immediately.
- Incorporate lifestyle habits that support oral and systemic health.
Patients with dental implant Manchester restorations, including subperiosteal options, benefit from long-term monitoring to ensure their implants remain secure and free from inflammation-related complications.
Conclusion
Inflammation is a silent but significant threat to the success of subperiosteal dental implants. Understanding its causes, recognising early signs, and implementing preventive measures can protect the soft tissues and ensure implant longevity. Maintaining oral hygiene, professional monitoring, and lifestyle adjustments are all critical components of a successful long-term strategy.At Smilo Dental Implant Manchester, our team combines expertise, technology, and personalised care to manage inflammation risks effectively. By prioritising tissue health alongside advanced implant techniques, we help patients achieve durable, aesthetically pleasing, and fully functional smiles that last a lifetime.




