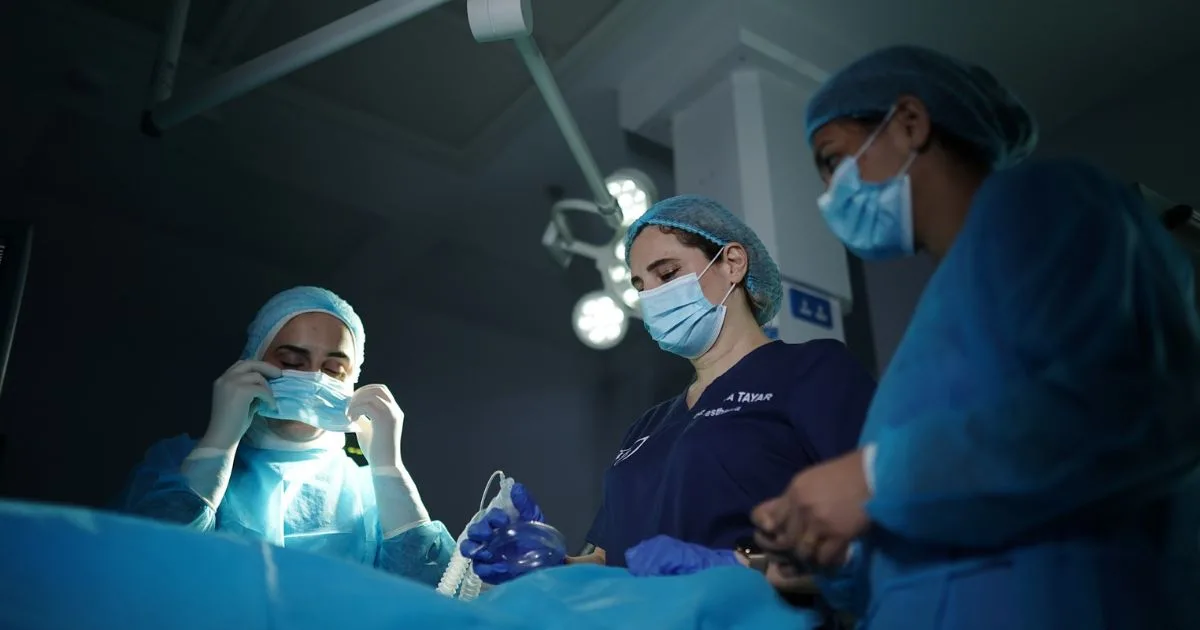
This article discusses GLP-1 medicines and gestational diabetes. The specifics of how tirzepatide works and the associated risks of using it during pregnancy are provided. There is also information on the link between obesity and gestational diabetes, along with an explanation of how early treatment will help improve long-term health outcomes.
Key Takeaways
- GLP-1 Medicines help manage blood sugar by improving insulin release, slowing digestion, and reducing appetite.
- Tirzepatide and Mounjaro 2.5mg Injection require strict medical supervision, especially during pregnancy.
- Obesity directly raises the risk of gestational diabetes by causing insulin resistance.
- Managing gestational diabetes well can significantly prevention type 2 diabetes later.
Gestational Diabetes can negatively impact the mother and baby if not treated properly. When diagnosed early in pregnancy, with proper lifestyle changes and treatment approach, the mother and/or baby may have an easier time during pregnancy with fewer complications.
What Is Gestational Diabetes and Why Does It Matter?
Gestational Diabetes is the diabetes that pregnant mothers develop because the insulin that their body produces does not work correctly at that time, resulting in high levels of sugar (glucose) in the blood and possible negative effects on the mother and/or baby.
Pregnancy hormones can interfere with the function of insulin by decreasing its effectiveness, leading to the development of gestational diabetes. The pancreas will continue to produce insulin; however, the body has difficulty using it correctly. Insulin resistance will cause elevated blood sugar levels. If elevated blood sugar levels are not managed very carefully, it will put both the baby and the mother at risk for serious complications.
- Symptoms of gestational diabetes include Thirst, frequent urination, fatigue, blurry vision, and sugar in your urine.
- And prevention tips include eating healthy foods, maintaining a healthy weight, being active, and receiving prenatal care (regular doctor visits during pregnancy).
- After being diagnosed with gestational diabetes, you can change the way you live or get treatment. These actions will help you and your baby have a better outcome.
What Are GLP-1 Medicines and How Do They Work?
GLP-1 medicines mimic a natural hormone that the gut releases after eating. That hormone tells the pancreas to release insulin when blood sugar rises, and slows digestion. Hence, glucose enters the bloodstream gradually, signalling the brain that the body has eaten enough.
- They reduce post-meal blood sugar spikes by slowing glucose absorption.
- They don't require daily dosing, unlike many older diabetes medicines.
- They work alongside diet and lifestyle changes, not instead of them.
- A doctor always assesses suitability before prescribing.
How Does Tirzepatide Work Differently?
Most GLP-1 Medicines target one receptor. Tirzepatide targets two: GIP and GLP-1. That dual action produces a broader and more consistent effect on blood sugar control. Many patients respond to it when single-receptor medicines haven't delivered enough improvement.
Tirzepatide also produces meaningful weight loss alongside blood sugar management, which matters particularly for women managing obesity alongside gestational diabetes. Its use during pregnancy, however, remains subject to limited safety data and requires careful medical assessment before any prescription is considered.
- It activates both GIP and GLP-1 receptors simultaneously.
- Blood sugar control tends to be more consistent than with single-receptor treatments.
- Weight reduction is a well-documented additional benefit outside of pregnancy.
- It's prescribed only when a doctor determines it's appropriate for the patient's specific health situation.
What is Mounjaro 2.5mg Injection and Who Is It For?
The Mounjaro 2.5mg injection contains tirzepatide at its lowest dose, with your doctor starting patients at this dose so that the body can adapt to the medication before trying a higher amount. Starting at a low level reduces the risk of side effects such as nausea and minor stomach upset.
It is administered at home with a prefilled pen once a week, and most people use the device without issues after the first use. Your doctor will consider your complete medical history when prescribing for you and will continue to monitor how well the drug is working for you.
Whether or not you should take this drug during pregnancy is completely up to your physician. This drug is not currently recommended by any national guidelines to be used routinely in pregnant females with diabetes, and there is not enough information currently available to support this drug as safe during pregnancy. If you are considering this drug, you should speak with your physician first.
How Does Obesity Increase the Risk of Gestational Diabetes?
It is significant to understand that obesity causes gestational diabetes. Gaining too much. body weight requires the body to produce more insulin to maintain an appropriate blood sugar level (blood glucose) because excess fat causes insulin resistance, the body's inability to utilise insulin.
- Gaining too much excess fat in the body can cause insulin resistance, even before pregnancy has begun.
- Some of the signs of obesity are continued fatigue, excessive thirst, and difficulty regulating weight.
- Prevention measures: Healthy diet, Regular exercise, Preconception health checkups.
- Having a lower body weight before pregnancy increases insulin sensitivity and reduces the risk of gestational diabetes.
How Does Managing Gestational Diabetes Help Prevent Type 2 Diabetes Later?
Women who experience gestational diabetes are at a higher risk of developing type 2 diabetes within 10 years of delivering their child. Even though the risk is real, it is greatly reduced with consistent action. Maintaining stable blood sugar during pregnancy protects the pancreas and helps maintain high insulin sensitivity, establishing healthy habits that will continue into daily life after the child arrives.
- Staying active and eating healthy after giving birth helps maintain the body's insulin response.
- Regular annual blood tests to monitor blood sugar levels can help identify early signs of changing blood sugar levels.
- Making consistent lifestyle choices after pregnancy contributes more to a woman's long-term health.
Final Thought
Gestational diabetes needs timely care, regular monitoring, and the right medical guidance to protect both mother and baby. With healthy lifestyle choices, expert support, and prescribed treatments when needed, women can manage blood sugar safely during pregnancy and lower future risks of developing type 2 diabetes.
Disclaimer: This blog is for informational purposes only and does not substitute for professional medical advice, diagnosis, or treatment. Always consult a qualified healthcare professional before making any decisions about medication or care during pregnancy.