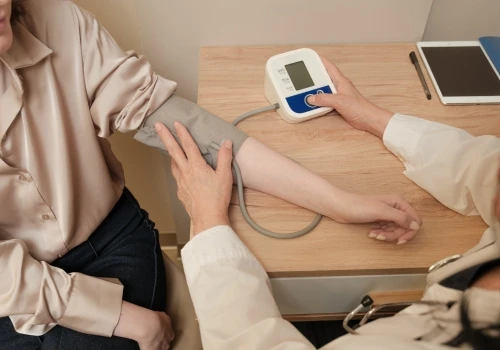
Blood pressure is a key indicator of cardiovascular health. While high blood pressure often receives more attention, a sudden or chronic decrease in blood pressure can also signal underlying health issues. Recognizing when blood pressure drops and understanding its causes is essential for maintaining heart health and overall well-being.
For individuals experiencing dizziness, fainting, or unexplained fatigue, learning about blood pressure decrease causes can help identify potential triggers and determine whether medical evaluation is necessary.
YouTube Link: https://youtu.be/S063HjXiiyE
Common Causes of Blood Pressure Drops
Low blood pressure, also called hypotension, can occur due to a variety of factors:
- Dehydration: Inadequate fluid intake can reduce blood volume.
- Medications: Certain heart medications, diuretics, or vasodilators may lower blood pressure.
- Heart conditions: Issues such as bradycardia, heart valve problems, or heart failure can reduce cardiac output.
- Endocrine disorders: Conditions like thyroid disease or adrenal insufficiency can influence blood pressure.
- Severe infections or blood loss: Acute medical events may trigger sudden hypotension.
Understanding the underlying cause is crucial to prevent complications and guide appropriate treatment.

When Low Blood Pressure Becomes Concerning
While mild hypotension may be manageable, it becomes concerning when it causes noticeable symptoms or indicates an underlying problem. Warning signs include:
- Dizziness, lightheadedness, or fainting
- Blurred vision
- Fatigue or weakness
- Nausea
- Rapid, shallow breathing or confusion
If these symptoms appear, it is important to seek timely evaluation to prevent falls, injuries, or organ damage.
Supporting Healthy Circulation
Maintaining strong circulation can help manage both low and high blood pressure. For example, leg circulation issues like varicose veins can be alleviated using support socks for varicose veins. Improved leg circulation can reduce strain on the cardiovascular system and help stabilize blood pressure.
In addition, heart rhythm irregularities such as palpitations can affect blood pressure. Knowing when to worry about heart palpitations helps patients understand when to seek immediate care.
Peripheral Artery Disease and Blood Flow
Peripheral artery disease (PAD) can also contribute to circulatory issues. Reduced blood flow due to narrowed arteries can worsen symptoms associated with low blood pressure, such as fatigue and cold extremities. For some patients, peripheral artery disease medical procedures may be recommended to restore circulation and improve overall cardiovascular health.
Signs of PAD include:
- Leg pain or cramping during activity
- Numbness or weakness
- Cold or discolored extremities
Early diagnosis and intervention can prevent severe complications and improve quality of life.
Lifestyle Tips for Managing Blood Pressure
Several habits can help maintain stable blood pressure and support cardiovascular health:
- Stay hydrated and consume adequate fluids daily
- Eat a balanced diet with sufficient electrolytes
- Avoid sudden changes in posture, especially when standing up quickly
- Exercise regularly to strengthen the heart and improve circulation
- Monitor blood pressure at home and track changes over time
Combined with professional care, these measures can help reduce the risk of complications from hypotension.
YouTube Link: https://youtu.be/4OsRcoZNGF8
Final Thoughts
Low blood pressure can sometimes indicate an underlying medical issue or develop suddenly due to lifestyle factors or heart conditions. Recognizing symptoms, understanding potential causes, and seeking timely evaluation are critical for maintaining cardiovascular health. Cypress Cardiovascular Institute, with locations in Cypress and Houston, offers expert evaluation and treatment for blood pressure concerns, circulatory issues, PAD, and heart rhythm disorders.