Varicose veins in feet develop when weakened vein valves allow blood to pool rather than flow efficiently back to the heart. While varicose veins most commonly appear in the legs, they can extend into the feet and create distinct podiatric complications that require specialized foot care.
Understanding how venous insufficiency affects your feet helps you recognize when foot-specific symptoms require podiatric evaluation rather than general vascular care alone.
What Are Varicose Veins in Feet?
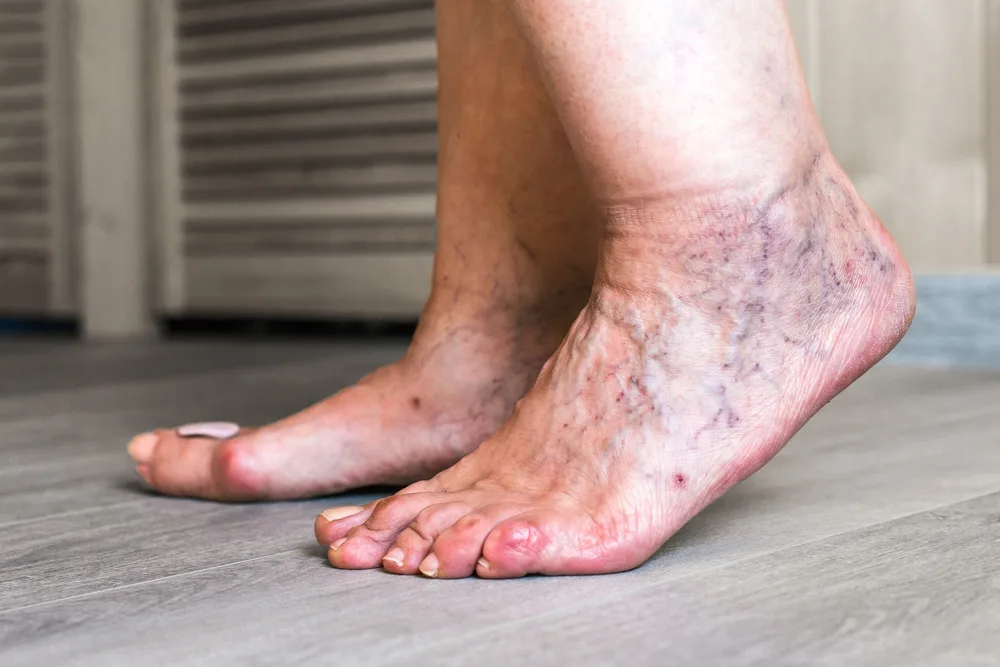
Varicose veins in feet are enlarged, twisted veins visible beneath the skin on the foot and ankle. They form when vein valves malfunction, allowing blood to flow backward and pool.
These veins typically appear blue or purple and may create raised, rope-like textures on the top of the foot or around the ankle. While spider veins—smaller, web-like veins—are primarily cosmetic, true varicose veins in the feet often signal underlying venous insufficiency requiring medical attention.
The foot contains numerous superficial veins that normally return blood from the toes and foot surface toward larger leg veins. When these pathways become impaired, blood accumulates in foot tissues, creating both visible vein changes and functional symptoms.
What Causes Varicose Veins in Feet?
Varicose veins develop when vein valves weaken or fail. Gravity pulls blood downward toward the feet, and healthy valves prevent backflow by closing after each heartbeat.
When valves malfunction, blood pools in lower extremity veins, increasing pressure and stretching vein walls. This creates the characteristic enlarged, twisted appearance of varicose veins.
Risk Factors for Developing Varicose Veins
Several factors increase your risk of developing varicose veins in feet:
- Age — Vein valves naturally weaken over time, making varicose veins more common after age 50
- Prolonged standing or sitting — Occupations requiring extended time on your feet or seated limit circulation and increase vein pressure
- Pregnancy — Increased blood volume and hormonal changes relax vein walls
- Obesity — Excess weight places additional pressure on leg and foot veins
- Family history — Genetic predisposition significantly increases varicose vein risk
- Previous leg injuries or blood clots — Prior vascular damage impairs normal vein function
Symptoms of Varicose Veins in Feet
Beyond visible purple veins or enlarged vessels, varicose veins in feet produce distinct symptoms that affect daily function and comfort.
Early Stage Symptoms
Initial symptoms often include:
- Aching or heaviness in feet — particularly after prolonged standing
- Mild swelling around ankles and top of foot — worsens throughout the day
- Burning or tingling sensations — especially at night
- Visible spider veins or small purple veins — web-like patterns on foot surface
These early symptoms often improve with elevation, compression, or rest, but they typically worsen over time without treatment.
Advanced Symptoms and Complications
Untreated varicose veins can progress to more serious foot complications:
- Skin changes — Discoloration, thickening, or leathery texture on feet and ankles
- Venous stasis dermatitis — Itchy, inflamed skin that may crack or weep fluid
- Venous ulcers — Open sores, typically near the ankle or on the foot, that heal slowly
- Persistent swelling — Chronic edema that doesn't resolve with elevation
- Foot pain that limits walking — Severe varicose vein pain affecting mobility
These complications require coordinated care between vascular specialists and podiatrists to address both the underlying venous insufficiency and the foot-specific issues.
How Podiatrists Manage Foot Complications from Varicose Veins
Podiatrists treat foot-related complications of venous insufficiency while coordinating with vascular specialists who address the underlying vein disease.
This collaborative approach ensures both the vascular cause and the foot symptoms receive appropriate care.
Conservative Foot Care Strategies
Podiatrists recommend several conservative measures to manage foot symptoms:
- Compression therapy — Medical-grade compression stockings reduce swelling and improve blood flow from feet back toward the heart
- Elevation — Raising feet above heart level for 15-20 minutes several times daily helps drain pooled blood
- Activity modification — Regular movement breaks during prolonged sitting or standing prevent blood stagnation
- Proper footwear — Supportive shoes with adequate room reduce pressure on swollen feet
These strategies manage symptoms but do not treat the underlying venous insufficiency. Patients often need both podiatric care and vascular treatment for comprehensive management.
Treatment for Skin Changes and Ulcers
When varicose veins cause skin complications, podiatrists provide specialized wound care:
- Wound debridement — Removal of dead tissue to promote healing
- Specialized dressings — Moisture-balancing materials that protect ulcers and support tissue regeneration
- Infection management — Topical or oral antibiotics when bacterial infection complicates venous ulcers
- Offloading techniques — Custom orthotics or padding to reduce pressure on ulcer sites
Venous ulcers heal slowly and often recur without addressing the underlying vein disease. Podiatrists coordinate with vascular surgeons to ensure patients receive both wound care and vein treatment.
When to See a Podiatrist for Varicose Veins in Feet
Schedule a podiatry consultation if you experience foot-specific symptoms that interfere with daily activities or show signs of skin complications.
Red Flag Symptoms Requiring Immediate Evaluation
Seek prompt podiatric care if you develop:
- Open sores or ulcers on feet or ankles — Especially if they fail to heal within two weeks
- Skin discoloration or thickening — Brown, reddish, or dark purple patches around varicose veins
- Persistent swelling despite elevation — Chronic edema that worsens over time
- Severe foot pain that limits walking — Varicose vein pain affecting mobility and quality of life
- Signs of infection — Warmth, redness, increasing pain, or drainage from skin lesions
These symptoms indicate advanced venous insufficiency complications requiring professional intervention. Early treatment prevents progression to more serious conditions.
Prevention Strategies: How to Prevent Varicose Veins in Feet
While genetic factors influence varicose vein development, lifestyle modifications reduce risk and slow progression in those already affected.
- Maintain healthy weight — Reducing excess pounds decreases pressure on leg and foot veins
- Exercise regularly — Walking, swimming, and cycling strengthen calf muscles that pump blood from feet back to the heart
- Avoid prolonged standing or sitting — Take movement breaks every 30-60 minutes to prevent blood pooling
- Elevate feet when resting — Raising feet above heart level improves circulation and reduces vein pressure
- Wear compression stockings — Medical-grade compression prevents blood from pooling in foot veins
- Choose supportive footwear — Low heels and shoes with good arch support promote healthy circulation
These prevention strategies are most effective when started early, before significant vein damage occurs. If you have a family history of varicose veins, implementing these habits proactively reduces your risk.
Varicose Vein Treatment Options
Treating the underlying venous insufficiency requires vascular specialist care. Common treatment options include:
- Sclerotherapy — Injection therapy that closes spider veins and small varicose veins
- Endovenous laser treatment (EVLT) — Laser energy seals larger varicose veins from inside
- Radiofrequency ablation — Heat-based closure of damaged veins
- Surgical vein stripping — Removal of severely damaged veins through small incisions
These treatments address the vein disease itself but do not manage foot-specific complications like ulcers or skin changes. Comprehensive care involves both vascular treatment and podiatric management.
If you're experiencing symptoms related to varicose veins in your feet, consult both a vascular specialist and a podiatrist. This coordinated approach ensures you receive complete care for both the underlying vein disease and the foot complications it causes.
Varicose veins in feet are more than a cosmetic concern. They signal venous insufficiency that can lead to serious foot complications including skin changes, ulcers, and chronic pain.
While vascular specialists treat the underlying vein disease through procedures like laser treatment and sclerotherapy, podiatrists manage the foot-specific symptoms and complications. This dual approach provides comprehensive care addressing both cause and effect.
Early intervention produces the best outcomes. If you notice purple veins, swelling, skin changes, or pain in your feet, seek professional evaluation from a board-certified podiatrist. Timely care prevents progression to advanced complications and improves your long-term foot health.