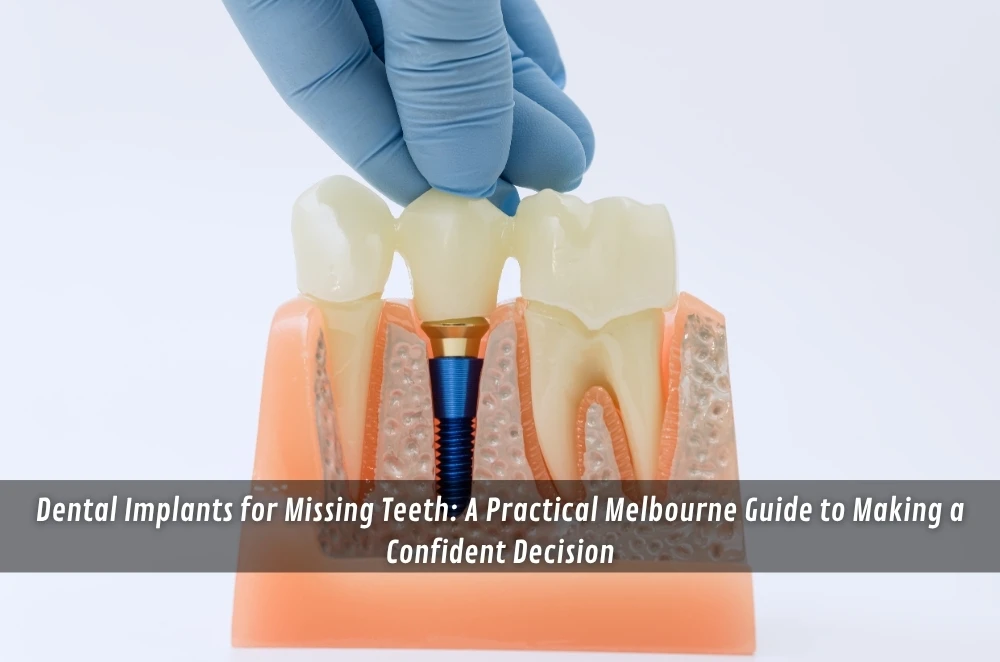
Missing teeth can do your head in a bit.
It’s not just about how it looks in photos—it can change how you chew, how you talk, and even which side you automatically use when you eat.
Dental implant treatment can be a solid option for replacing missing teeth, but it’s not a “bang it in and you’re done” situation.
If you’re in Melbourne and weighing it up, here’s a plain-English guide to help you make a call without getting swept up in hype.
Why it feels urgent (and why rushing can bite you later)
When a tooth has been gone for a while, people often panic that everything’s about to slide downhill.
Sometimes there are good reasons not to leave it forever, but rushing can lead to skipping the basics: proper assessment, realistic timeframes, and a plan that suits your health and budget.
A calm, step-by-step approach usually beats a fast decision made on a stressful day.
And if anyone makes it sound like there’s one “best” solution for everyone, take that with a grain of salt.
What dental implant treatment usually looks like
Implants are a process.
The exact steps vary, but most treatment plans follow a similar shape.
1) The assessment and planning bit
This is where medical history, oral health, and imaging come into it.
It’s also where the real options get laid out: implants, bridges, dentures, or sometimes stabilising other issues first and coming back to replacement.
If gum disease or decay is active, that can change what’s sensible to do first.
2) Preparing the area (sometimes)
Some people have enough bone and gum support for a straightforward plan.
Others may need extra consideration—like bone grafting—or an alternative approach depending on the site and the overall mouth.
That’s not a failure; it’s just the reality of biology.
3) Placing the implant
The implant is usually a small titanium (or titanium-alloy) post placed into the jawbone.
Then comes healing time so it can integrate.
Some cases move quickly, others take longer, and a staged plan is common.
4) Fitting the tooth/teeth on top
After healing, the restoration is fitted (often a crown for a single tooth, or another design for multiple teeth).
The aim isn’t just “looks good”—it needs to fit the bite and be easy to clean.
If it’s a nightmare to keep clean, it’s not a great long-term setup.
Common mistakes people make (no judgement)
Most people aren’t doing anything “wrong”—they’re just trying to make a big decision with mixed info.
Here are the traps that pop up a lot.
Mistake 1: Choosing based on speed alone
“Same-day” language can sound unreal when you just want your normal life back.
But not every mouth is suited to a fast-track plan, and chasing speed can mean compromises.
Sometimes the smarter plan is the one that’s a bit slower but more predictable.
Mistake 2: Thinking implants are “set and forget”
Implants can’t get tooth decay, but the gums around them still matter.
If cleaning is patchy, check-ups are irregular, or health factors aren’t managed, complications can happen.
It’s better to think of implants like a good car: reliable if you maintain it.
Mistake 3: Not asking what happens if the plan changes
Some plans change mid-stream: more healing time, different restoration choices, or staged steps.
Before committing, ask what the “Plan B” looks like if the site needs more preparation than expected.
Clarity early saves a lot of frustration later.
Mistake 4: Ignoring the whole-mouth picture
Replacing one missing tooth isn’t always isolated.
Bite pressure, grinding, neighbouring teeth, and gum health all affect how stable and comfortable the result will be.
A good plan explains how the implant fits with the bite and hygiene routine—otherwise you’re flying blind.
Mistake 5: Comparing outcomes, not effort
When comparing implants vs bridges vs dentures, people often focus on the final look.
A more useful comparison includes: number of appointments, healing time, cleaning effort, and likely maintenance.
Sometimes the best option is the one you can actually keep up with, week after week.
Decision factors that actually matter (not the marketing stuff)
If you’re considering dental implant treatment for missing teeth, these are the real-life factors worth weighing up.
General health and medications
Some conditions and medications can affect healing or surgical risk.
That doesn’t automatically rule implants out, but it can change timing or require coordination with a GP or specialist.
A simple move: bring an up-to-date medication list and ask how it affects the plan.
Bone support and how long the tooth’s been missing
After tooth loss, the site can change over time.
That doesn’t mean “too late”, but it may affect complexity and whether preparation steps are needed.
One tooth vs multiple teeth
Single tooth replacement is different to replacing a few.
With multiple missing teeth, there may be several ways to design the solution—aiming for stability and cleanability without making it impossible to maintain.
Budget (and the real cost over time)
Cost isn’t only the upfront number.
It’s also maintenance, check-ups, hygiene tools, and any future adjustments.
It’s fair to ask for costs in stages, because implant treatment is often staged.
Comfort, anxiety, and how treatment fits real life
For plenty of people, the biggest barrier is the experience, not the decision.
It’s okay to talk about anxiety and ask what support options are available.
And it’s smart to choose a provider who explains things clearly—no rushing, no pressure.
Questions to take into the consult
A consult is way more useful when you come in organised.
If it helps to walk in with your ducks in a row, bring a short list of priorities and questions—this High Dental Implants treatment guide can help you shape that list without overthinking it.
Keep it practical: suitability, steps, timeline, and what cleaning will look like day-to-day.
Operator Experience Moment
A common moment is when someone arrives convinced implants are the only answer, then feels rattled when trade-offs come up.
What usually helps is turning the whole thing into a simple sequence: stabilise what needs stabilising, confirm suitability, then replace teeth in an order that fits life and work.
Once there’s a timeline you can picture and a maintenance routine that feels doable, the decision stops feeling so heavy.
Local SMB Mini-Walkthrough (Melbourne)
A small café owner in Melbourne realises they’re chewing on one side and avoiding certain foods.
They book a consult early in the week so recovery doesn’t clash with the weekend rush.
They bring their medication list and ask what parts of the plan are fixed vs flexible.
They talk through a staged approach that works around staffing and long shifts on their feet.
They pick a cleaning routine that won’t fall apart during 5am starts.
They schedule follow-ups during quieter trading weeks so it’s not a drama.
A simple next-7-to-14-days plan (no heroics required)
The goal here isn’t to “lock in implants”.
It’s to get clear on what’s realistic and what’s not.
Days 1–3: Get your basics sorted
- Write down what’s actually bothering you (chewing, appearance, speech, shifting, discomfort).
- List medical conditions, meds, and any factors that might affect healing (including smoking/vaping).
- Note what stresses you out about dental treatment and what helps (breaks, clear explanations, music).
Days 4–7: Book the right type of consult
- Choose a consult that includes proper assessment and a discussion of alternatives.
- Ask what imaging or records are needed and whether they’re included.
- Prep 6–8 questions: suitability, steps, healing time, cleaning, and how plans change if surprises pop up.
Days 8–14: Compare like-for-like
- Compare at least two approaches if appropriate (implant vs bridge vs denture).
- Compare timelines and maintenance effort, not just the “final look”.
- If anything is unclear, ask for the staged plan in writing so you’re not relying on memory.
Practical Opinions
The best plan is usually the one you can maintain, not the one that sounds flash.
If the cleaning routine feels unrealistic, change the design before treatment starts.
Clear stages and contingencies beat chasing a perfect timeline every day of the week.
Key Takeaways
- Implant treatment is typically staged, and timelines vary depending on health and bone support.
- A good consult covers suitability, sequencing, and maintenance—not just the implant itself.
- Avoid rushing: speed-first decisions can create trade-offs you don’t need.
- Compare options by upkeep and effort as well as the end result.
- A simple 7–14 day plan can reduce uncertainty before committing.
Common questions we hear from Australian businesses
Q1) How long does implant treatment usually take for missing teeth?
It depends on healing needs and whether preparation steps are required, but in most cases it’s staged over months rather than weeks. A practical next step is to ask for a written timeline that shows each appointment and the decision points. In Melbourne, plenty of people plan treatment around work peaks, school terms, and the daily commute, so flexibility is worth discussing.
Q2) Are implants always better than a bridge or denture?
Usually, implants are a strong option, but they aren’t automatically the best fit for every mouth, budget, or lifestyle. A practical next step is to ask your clinician to compare options using the same criteria: cleanability, timeline, maintenance, and what happens if the plan changes. In most cases, Australians end up choosing the option they can keep up with alongside regular check-ups.
Q3) What if I’m nervous about the procedure or worried about pain?
In most cases, anxiety can be managed with a clear plan, communication preferences, and comfort options discussed in advance. A practical next step is to tell the clinic what you’re worried about and ask what support is available (clear step-by-step explanations, breaks, and sedation options where clinically suitable). In Melbourne, busy work weeks can crank stress up, so choosing appointment times that reduce pressure can make a big difference.
Q4) How do I know if I’m a candidate for implants?
It depends on overall health, gum condition, bone support, and how your bite functions, so it really needs an individual assessment. A practical next step is to book a consult and bring your full medication list and relevant medical history so the conversation is accurate. In most cases, getting clarity early helps—even if the best plan is staged or starts with preparation first.