 Introduction
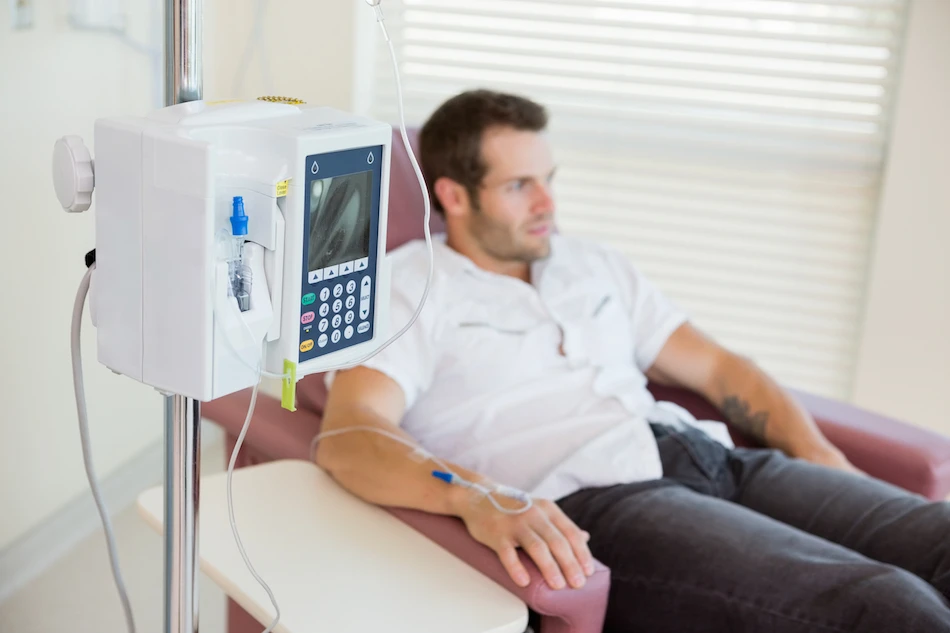
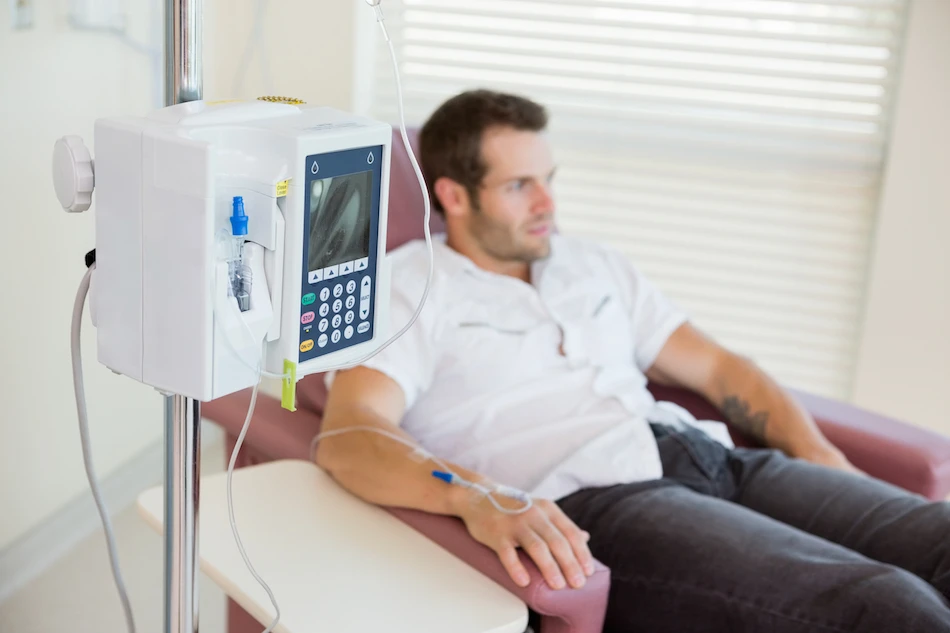
IntroductionChemotherapy is one of the most widely used and effective treatment modalities in the fight against cancer. It involves the use of potent drugs to destroy or slow the growth of cancer cells. This method is especially crucial in treating hematological cancers such as leukemia, lymphoma, and multiple myeloma. In the field of haemato-oncology, chemotherapy continues to be a cornerstone of therapy, often used alone or in combination with other treatments like radiation or stem cell transplantation.
Chemotherapy refers to the use of anti-cancer (cytotoxic) drugs that target rapidly dividing cells in the body. Since cancer cells grow and divide faster than most normal cells, these drugs are designed to either kill these cells or stop them from multiplying. However, because some normal cells (like those in the hair, bone marrow, and digestive tract) also divide quickly, they can be affected as well — leading to side effects.
Chemotherapy drugs work by interfering with the cancer cells’ ability to divide and multiply. Some drugs damage the cell’s DNA during replication, while others inhibit the process of cell division. Depending on the type of cancer and its stage, doctors may use a single chemotherapy drug or a combination of drugs to achieve better results.
Chemotherapy can be categorized based on its intended goal:
- Aims to eliminate cancer completely and restore normal health.
- Given after surgery or radiation to kill any remaining cancer cells.
- Administered before surgery to shrink tumors, making them easier to remove.
- Used in advanced stages to relieve symptoms and improve quality of life, even if a cure is not possible.
Chemotherapy can be given in several ways, depending on the type of cancer and the specific drug used:
- Intravenous (IV): The most common method; drugs are infused directly into a vein.
- Oral (tablet or capsule form): Convenient for outpatient settings.
- Subcutaneous or intramuscular injections
- Intrathecal (into the cerebrospinal fluid): Used for cancers involving the brain or spinal cord.
- Topical (applied to the skin): Rare, for certain types of skin cancer.
Chemotherapy is usually given in cycles, with a rest period in between to allow the body to recover. A regimen may involve:
- Weekly, bi-weekly, or monthly cycles
- One or more drugs per cycle (combination chemotherapy)
- Duration ranging from a few months to a year, depending on disease response
The exact regimen is personalized based on cancer type, stage, patient health, and response to prior treatment.
Common Chemotherapy Drugs Used in Hematological Cancers- Leukemia: Cytarabine, Daunorubicin, Methotrexate
- Lymphoma: Cyclophosphamide, Doxorubicin, Vincristine, Prednisone (CHOP regimen)
- Myeloma: Melphalan, Bortezomib, Thalidomide, Lenalidomide
Each of these drugs has unique mechanisms of action and is selected based on disease subtype and patient profile.
Side Effects of ChemotherapyWhile chemotherapy is effective, it also affects healthy cells that divide rapidly. This leads to side effects, which vary by individual and the type of drugs used:
- Hair loss
- Fatigue and weakness
- Nausea and vomiting
- Diarrhea or constipation
- Loss of appetite
- Mouth sores
- Increased risk of infections
- Anemia and low platelet count
- Skin and nail changes
- Neuropathy (tingling in hands and feet)
These side effects are often temporary and manageable with supportive care.
Managing Side EffectsProper management can greatly reduce discomfort during chemotherapy:
- Anti-nausea medications to control vomiting
- Growth factors (e.g., G-CSF) to boost white blood cell counts
- Blood transfusions in case of severe anemia
- Nutritional support to maintain body strength
- Pain relief and antibiotics as needed
- Psychological support to cope with emotional distress
Patients should communicate openly with their healthcare team about any new or worsening symptoms.
Life During Chemotherapy: Tips for PatientsLiving with chemotherapy involves some lifestyle adjustments to reduce side effects and improve treatment outcomes:
- Stay well-hydrated
- Eat a balanced, nutritious diet
- Avoid crowds and sick individuals to reduce infection risk
- Get adequate rest and sleep
- Practice gentle physical activity like walking
- Maintain good oral hygiene
- Follow scheduled lab tests and doctor visits
In haemato-oncology, chemotherapy is often the first line of treatment. Unlike solid tumors, many blood cancers respond exceptionally well to systemic chemotherapy since these cancers affect circulating cells throughout the body.
- Acute leukemia: Intensive induction chemotherapy followed by consolidation
- Non-Hodgkin’s Lymphoma: CHOP or R-CHOP regimen for curative intent
- Multiple Myeloma: Induction chemotherapy before autologous stem cell transplant
In many cases, chemotherapy is combined with immunotherapy, targeted therapy, or stem cell transplantation to improve results.
Monitoring and Follow-upThroughout treatment, regular blood tests and imaging studies help assess how well chemotherapy is working. Adjustments to drug dosage or schedule may be made based on response or side effects. Post-treatment follow-up is crucial to monitor remission status and catch any signs of recurrence early.
Chemotherapy is not just a physical challenge — it can be mentally and emotionally taxing. Patients may experience anxiety, depression, or fear about the treatment and its outcome. Psychological counseling, patient support groups, and open family communication can help patients stay positive and resilient.
Chemotherapy remains a powerful and proven method in the treatment of cancer, especially in hematological malignancies. With advancements in drug development, side effect management, and personalized medicine, patients are experiencing better outcomes and improved quality of life. While it may come with challenges, chemotherapy offers hope and healing for many battling cancer today.