Introduction
Bone marrow or stem cell transplantation is a critical medical procedure used to treat various types of blood cancers and life-threatening hematologic conditions. It involves the replacement of damaged or destroyed bone marrow with healthy stem cells that can regenerate normal blood cells. This therapy has become a cornerstone in the treatment of diseases like leukemia, lymphoma, myeloma, aplastic anemia, and certain genetic disorders.
In this blog, we will explore what a stem cell transplant is, the different types, the procedure, indications, benefits, risks, and what patients can expect before, during, and after treatment.
What is Bone Marrow?
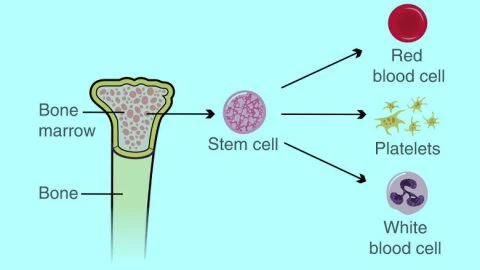
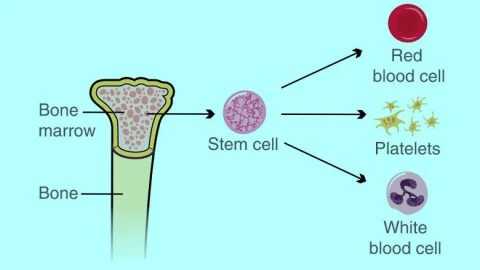
Bone marrow is the soft, spongy tissue found inside bones, primarily in the hip and thigh bones. It is responsible for producing blood-forming stem cells, which develop into:
- Red blood cells (carry oxygen)
- White blood cells (fight infection)
- Platelets (help blood clot)
When bone marrow is damaged by disease, chemotherapy, or a genetic condition, it may not produce healthy blood cells. A bone marrow or stem cell transplant becomes essential in such cases.
What is a Stem Cell Transplant?
A stem cell transplant is a medical procedure where a patient receives healthy stem cells to replace the diseased or damaged ones. These stem cells may come from the patient themselves (autologous) or from a donor (allogeneic).
The transplant helps the body:
- Rebuild a healthy blood and immune system
- Tolerate higher doses of chemotherapy or radiation
- Potentially cure certain blood cancers
Types of Stem Cell Transplants
1. Autologous Transplant
- Stem cells are collected from the patient before high-dose chemotherapy and then returned afterward.
- Common in multiple myeloma and lymphoma.
- Lower risk of immune complications like GvHD.
2. Allogeneic Transplant
- Stem cells come from a matched donor — usually a sibling or unrelated donor with compatible tissue type (HLA match).
- Used in leukemia, aplastic anemia, MDS, and genetic disorders.
- Carries risk of graft-versus-host disease (GvHD), but also offers graft-versus-leukemia (GvL) effect.
3. Haploidentical Transplant
- A newer approach using a half-matched family member (parent, child).
- Offers more donor availability.
4. Umbilical Cord Blood Transplant
- Stem cells collected from donated umbilical cords.
- Useful for pediatric or smaller adult patients.
Diseases Treated with Bone Marrow/Stem Cell Transplant
Stem cell transplantation is used in both malignant and non-malignant conditions, including:
Malignant Conditions (Blood Cancers):
- Leukemia (ALL, AML, CML, CLL)
- Lymphoma (Hodgkin and Non-Hodgkin)
- Multiple Myeloma
- Myelodysplastic Syndromes (MDS)
Non-Malignant Conditions:
- Aplastic Anemia
- Thalassemia major
- Sickle Cell Disease
- Severe Combined Immunodeficiency (SCID)
- Fanconi Anemia
- Congenital Neutropenia
The Stem Cell Transplant Process
Step 1: Pre-Transplant Evaluation
Patients undergo comprehensive tests to assess organ function, infection status, disease stage, and donor compatibility.
Step 2: Stem Cell Collection
- In autologous transplant, the patient’s own stem cells are mobilized using G-CSF injections and collected through a process called apheresis.
- In allogeneic transplant, stem cells are collected from the donor.
Step 3: Conditioning (Chemotherapy/Radiation)
High-dose chemotherapy (sometimes with radiation) is given to:
- Destroy diseased bone marrow
- Suppress the immune system to reduce rejection
Step 4: Stem Cell Infusion
Collected stem cells are infused into the bloodstream like a blood transfusion. These cells migrate to the bone marrow and begin to regenerate blood cells (engraftment).
Step 5: Post-Transplant Monitoring
Patients are closely monitored for infections, engraftment success, and transplant-related complications.
Recovery and Engraftment
Engraftment is the process by which the transplanted stem cells begin to grow and produce new blood cells. It usually takes:
- Neutrophils: ~10–21 days
- Platelets: ~2–3 weeks
- Red cells: Up to 6 weeks or more
During this time, patients are highly vulnerable to infections and require protective isolation, antibiotics, and supportive care.
Benefits of Stem Cell Transplantation
✅ Potential cure for many blood cancers and disorders
✅ Allows intensive chemotherapy that would otherwise be too toxic
✅ Restores immune function
✅ Reduces long-term dependence on blood transfusions
✅ Provides graft-versus-tumor effect in some cancers
Risks and Complications
Despite its benefits, a stem cell transplant carries risks that vary depending on the patient’s age, overall health, disease status, and donor match.
Short-term Risks:
- Nausea and vomiting
- Mucositis (mouth sores)
- Infections (bacterial, viral, fungal)
- Organ toxicity (liver, lungs, kidneys)
Long-term Risks:
- Graft-versus-host disease (GvHD)
- Fertility issues
- Secondary cancers
- Hormonal imbalances
- Delayed immune recovery
GvHD occurs when donor immune cells attack the recipient’s tissues, most commonly the skin, liver, and gut. It is managed using steroids and immunosuppressants.
Life After Transplant
Follow-Up Care Includes:
- Regular blood tests and bone marrow biopsies
- Preventive antibiotics and antifungals
- Vaccinations (as immunity needs to be rebuilt)
- Monitoring for GvHD, infections, or relapse
Patients are advised to:
- Avoid crowds and infections
- Eat hygienic, protein-rich diets
- Practice excellent hygiene
- Avoid strenuous activity for several months
Psychological and Emotional Aspects
A stem cell transplant is not just physically taxing — it can be emotionally overwhelming. Patients may experience anxiety, depression, or fatigue. Support groups, psychological counseling, and family support play a vital role in recovery.
Success Rates and Outcomes
Outcomes have improved significantly with advances in:
- HLA typing and donor matching
- Infection control
- Conditioning regimens
- GvHD prophylaxis
Success rates vary depending on disease type, stage, donor match, and age. For example:
- Autologous transplants for myeloma or lymphoma often have success rates of 70–80%
- Allogeneic transplants for leukemia have variable outcomes based on risk profile
Future of Stem Cell Transplantation
The field is evolving rapidly, with ongoing research focused on:
- Improving donor availability through haploidentical transplants and cord blood
- Reducing GvHD with selective T-cell manipulation
- Safer conditioning regimens
- Gene therapy combined with stem cell transplantation (e.g., for sickle cell and thalassemia)
- CAR-T cell therapy as an alternative or adjunct
Conclusion
Bone marrow or stem cell transplantation is a life-saving therapy for patients with serious blood cancers and disorders. Though it is a complex procedure with potential complications, it offers hope for a cure or long-term remission in conditions that were once considered incurable. With ongoing medical advances and supportive care, more patients are benefiting from this transformative treatment every year.