Introduction
When it comes to heart and blood vessel health, most people focus on heart attacks and strokes. However, there’s another serious yet often overlooked condition that deserves attention—Peripheral Arterial Disease (PAD). This condition affects millions of people worldwide, yet many remain unaware of its early warning signs.
Peripheral Arterial Disease occurs when arteries that supply blood to the limbs—especially the legs—become narrowed due to plaque buildup. As a result, blood flow is restricted, leading to discomfort, pain, and in severe cases, tissue damage.
If left untreated, PAD can significantly impact your quality of life and even increase the risk of life-threatening complications. That’s why understanding its symptoms, causes, and treatment options is crucial.
For a deeper understanding and expert care, visit this comprehensive guide on Peripheral Arterial Disease (PAD).
What is Peripheral Arterial Disease (PAD)?
Peripheral Arterial Disease is a circulatory condition caused by atherosclerosis—a buildup of fatty deposits (plaque) in the arteries. This buildup reduces blood flow to the limbs, particularly the legs.
Unlike sudden conditions, PAD develops gradually over time. Many people may not notice symptoms in the early stages, making it even more dangerous. As the disease progresses, reduced blood flow can lead to pain, mobility issues, and even non-healing wounds.
Common Symptoms of PAD
One of the biggest challenges with PAD is that symptoms can be mild or easily ignored. However, recognizing early signs can make a huge difference.
1. Leg Pain While Walking (Claudication)
This is the most common symptom. You may feel cramping or pain in your legs or hips while walking, which usually disappears after rest.
2. Numbness or Weakness
Reduced blood flow can cause your legs to feel weak or numb, especially after physical activity.
3. Coldness in Lower Limbs
One leg or foot may feel colder than the other due to poor circulation.
4. Slow-Healing Wounds
Cuts or sores on your feet or legs that take longer to heal may indicate reduced blood supply.
5. Changes in Skin Color
Your skin may appear pale, bluish, or shiny due to inadequate oxygen supply.
6. Hair Loss on Legs
Decreased blood flow can also lead to reduced hair growth on your legs and feet.
Causes of Peripheral Arterial Disease
The primary cause of PAD is atherosclerosis. However, several lifestyle and health factors contribute to its development:
1. Smoking
Smoking is one of the leading causes of PAD. It damages blood vessels and accelerates plaque buildup.
2. Diabetes
High blood sugar levels can damage blood vessels over time, increasing the risk of PAD.
3. High Blood Pressure
Hypertension puts extra strain on arteries, making them more prone to narrowing.
4. High Cholesterol
Excess cholesterol contributes to plaque formation in arteries.
5. Obesity
Being overweight increases the risk of developing vascular diseases, including PAD.
6. Sedentary Lifestyle
Lack of physical activity reduces circulation and overall cardiovascular health.
Who is at Risk?
Certain individuals are more likely to develop Peripheral Arterial Disease:
- People over 50 years of age
- Smokers or former smokers
- Individuals with diabetes
- Those with a family history of cardiovascular disease
- People with high cholesterol or hypertension
Understanding your risk factors can help you take preventive measures early.
Why PAD Should Not Be Ignored
Ignoring PAD can lead to serious complications:
1. Critical Limb Ischemia
Severely reduced blood flow can cause chronic pain, infections, and even tissue death.
2. Increased Risk of Heart Attack and Stroke
PAD is often a sign of widespread atherosclerosis, meaning other arteries (including those supplying the heart and brain) may also be affected.
3. Reduced Mobility
Persistent leg pain can limit your ability to walk or perform daily activities.
Early diagnosis and treatment are essential to prevent these outcomes.
Diagnosis of Peripheral Arterial Disease
Doctors use several methods to diagnose PAD:
1. Physical Examination
Checking pulses in the legs and feet.
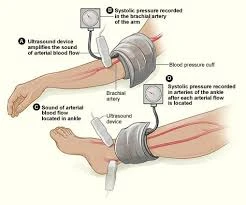
2. Ankle-Brachial Index (ABI)
A simple test comparing blood pressure in the ankle and arm.
3. Ultrasound Imaging
Helps visualize blood flow in arteries.
4. Angiography
Provides detailed images of blocked or narrowed arteries.
These diagnostic tools help determine the severity of the condition and guide treatment.
Treatment Options for PAD
The good news is that PAD is manageable, especially when detected early. Treatment focuses on improving blood flow and reducing symptoms.
1. Lifestyle Changes
Quit Smoking
This is the most important step in slowing disease progression.
Regular Exercise
Walking programs can significantly improve symptoms and circulation.
Healthy Diet
A balanced diet helps control cholesterol, blood pressure, and weight.
2. Medications
Doctors may prescribe medications to:
- Lower cholesterol levels
- Control blood pressure
- Prevent blood clots
- Manage blood sugar in diabetic patients
3. Minimally Invasive Procedures
For more severe cases, doctors may recommend:
Angioplasty
A small balloon is used to open narrowed arteries.
Stenting
A mesh tube is placed in the artery to keep it open.
4. Surgical Options
In advanced cases, bypass surgery may be performed to redirect blood flow around blocked arteries.
Preventing Peripheral Arterial Disease
Prevention is always better than cure. Here are some simple yet effective steps:
- Quit smoking
- Stay physically active
- Maintain a healthy weight
- Monitor blood pressure and cholesterol
- Manage diabetes effectively
- Eat a heart-healthy diet
Making these changes not only prevents PAD but also improves overall cardiovascular health.
Living with PAD: Practical Tips
Managing PAD doesn’t mean giving up your lifestyle. With proper care, you can lead a healthy and active life.
- Follow your doctor’s treatment plan
- Stay consistent with medications
- Wear comfortable footwear
- Inspect your feet regularly for wounds
- Avoid sitting or standing for long periods
Consistency is key to managing symptoms and preventing complications.
When to See a Doctor
You should seek medical attention if you experience:
- Persistent leg pain while walking
- Non-healing wounds on your legs or feet
- Sudden changes in skin color or temperature
- Numbness or weakness in your limbs
Early consultation can prevent serious complications and improve outcomes.
Conclusion
Peripheral Arterial Disease (PAD) is a serious yet manageable condition that often goes unnoticed until it becomes advanced. By understanding its symptoms, causes, and risk factors, you can take proactive steps toward early detection and effective treatment.
The key lies in awareness and timely action. Whether it’s adopting a healthier lifestyle, seeking medical advice, or following a treatment plan, every step counts in protecting your vascular health.
If you suspect any symptoms or fall into a high-risk category, don’t delay—early intervention can make all the difference in maintaining mobility, preventing complications, and improving your overall quality of life.