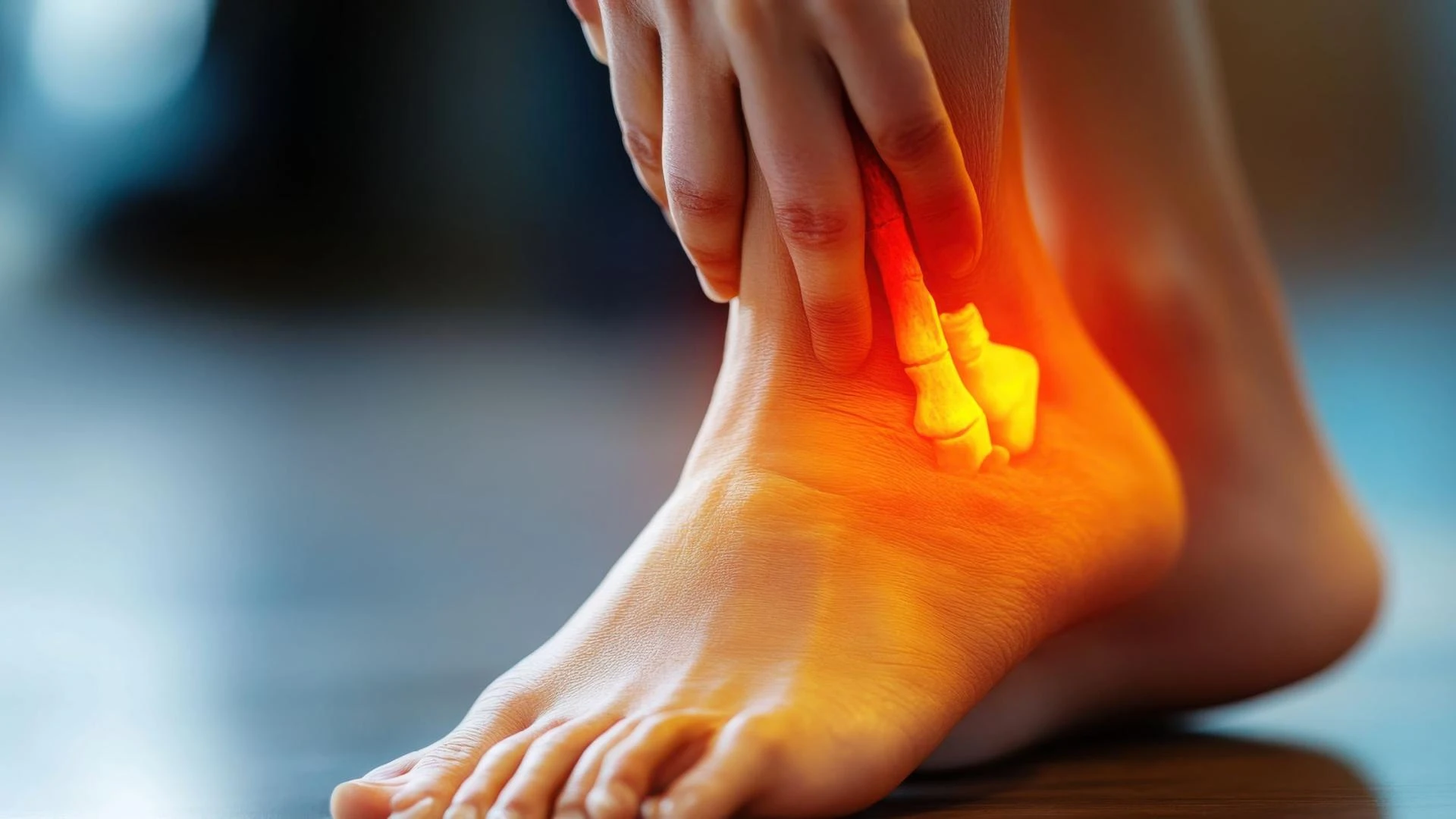
Chronic inflammation has quietly become one of the most significant health challenges of our time. Unlike the occasional inflammation that accompanies a sprained ankle or an immune response to a transient infection, chronic inflammation persists day after day, month after month, eroding health from within. Many people find themselves grappling with symptoms that are hard to pin down — lingering fatigue, joint stiffness, unpredictable pain, low-grade fever, or even mood changes that seem immune to lifestyle adjustments.
For decades, treatments for chronic inflammation relied mostly on broad-spectrum anti-inflammatory drugs, lifestyle advice, and in some cases, immunosuppressive therapies for autoimmune conditions. While those strategies have their place, they don’t always address the deeper biological drivers of persistent inflammation. That’s where science is now expanding into more nuanced, targeted approaches — including the use of peptides.
In this article, we’ll explore how researchers and clinicians are using peptides for inflammation support and healing, why they’re effective, and what this emerging area of care may offer for people seeking recovery beyond traditional therapies.
What Is Chronic Inflammation — and Why It Matters
Inflammation is part of the body’s natural defense system. When you cut your skin, sprain your wrist, or come down with a virus, inflammation is the mechanism that recruits immune cells, isolates damaged tissue, and initiates repair. In those situations, inflammation is acute — powerful but short-lived, with a clear beginning and end.
Chronic inflammation, on the other hand, is persistent and often silent. It doesn’t turn on and off with an injury or infection; it lingers. Over time, prolonged inflammatory activity can affect nearly every system in the body — from joints and muscles to organs and neural networks. Research has linked chronic inflammation to a wide range of conditions, including cardiovascular disease, type 2 diabetes, neurodegenerative disorders, autoimmune diseases, and even certain forms of cancer.
Part of the problem is that chronic inflammation isn’t always obvious. It doesn’t always present with dramatic swelling or acute pain. Instead, it often shows up as persistent low-level discomfort, fatigue, mood instability, or recurring health complaints that don’t seem to respond fully to standard care. People may feel “off” for no clear reason — and traditional treatments may only offer partial relief.
This complexity is why understanding the root causes and biological underpinnings of inflammation is so important, and why clinicians are increasingly looking beyond generic anti-inflammatory solutions to find strategies that support the body’s own healing systems.
The Biology of Inflammation: A Deeper Look
To understand how peptides can play a role in inflammation management, it helps to grasp what’s happening at the cellular level.
Inflammation involves a complex network of signaling molecules, immune cells, and regulatory pathways. When an inflammatory trigger — such as tissue damage, infection, or cellular stress — activates the immune system, a cascade of chemical messengers (like cytokines and chemokines) signals immune cells to move to the affected area. These cells work to eliminate threats and begin the repair process.
In acute injury, this system functions efficiently: the inflammation resolves once the threat is neutralized and healing begins. In chronic inflammation, however, the signaling pathways remain active, and immune cells continue to release inflammatory mediators even in the absence of a clear threat. This persistent signaling can lead to ongoing tissue stress, cell dysfunction, and a host of downstream consequences that extend beyond the original trigger.
Traditional Approaches to Inflammation Relief
Historically, people seeking relief from chronic inflammation have relied on several common approaches. Some focus on lifestyle modifications, such as:
- Diet changes to reduce pro-inflammatory foods and increase anti-inflammatory nutrients
- Regular exercise to support metabolic and immune health
- Stress management through practices like mindfulness, yoga, or therapy
- Adequate sleep to regulate immune function
Other strategies include pharmaceutical anti-inflammatory medications such as NSAIDs (non-steroidal anti-inflammatory drugs), corticosteroids, or disease-modifying agents for autoimmune conditions. While these treatments can be effective, they also come with limitations, especially when used long term. NSAIDs, for example, may lead to gastrointestinal irritation, cardiovascular risks, or kidney stress when used chronically. Corticosteroids can suppress the immune system and cause metabolic side effects.
Furthermore, these traditional approaches don’t always address the signaling pathways and cellular processes that sustain inflammation over time. That’s one reason why people with chronic inflammatory conditions frequently find themselves cycling through treatments without achieving consistent relief.
Introducing Peptides: What They Are and How They Work
Peptides are short chains of amino acids — essentially the building blocks of proteins. In the body, peptides act as signaling molecules, telling cells how to behave. They influence processes like immune function, tissue repair, metabolic regulation, and cellular communication. Because of their role as biological messengers, peptides have become a focus of interest for people seeking targeted support for inflammation, recovery, and healing.
Unlike broad-spectrum anti-inflammatory drugs, which suppress inflammation broadly (and sometimes indiscriminately), certain peptides can interact with specific pathways. They help modulate immune responses, support tissue repair, and encourage regulatory processes that bring balance back to inflamed systems.
It’s worth emphasizing that peptides are not a magic bullet. They don’t simply switch off inflammation. Instead, they act as modulators — guiding the body’s natural processes in a way that helps reduce chronic overactivity in inflammatory signaling while supporting recovery and repair.
How Peptides Are Used to Support Inflammation and Healing
Peptide therapy in the context of inflammation generally falls into a few categories: those that influence immune signaling, those that support tissue repair, and those that help regulate metabolic or oxidative stress pathways. Let’s explore how each category contributes to inflammation management.
Peptides That Modulate Immune Signaling
Some peptides work by influencing cytokines and other immune-signaling molecules. Cytokines are essential for immune communication — they tell immune cells where to go, how strongly to respond, and when to stand down. In chronic inflammation, certain cytokines remain elevated, contributing to persistent inflammatory responses.
Specific peptides act as regulators in these pathways. They help recalibrate immune signaling by encouraging a more balanced profile of pro-inflammatory and anti-inflammatory cytokines. The result is often a reduction in sustained inflammatory signals, without completely shutting down essential immune function.
Peptides Supporting Tissue Repair
Inflammation is only part of the story. Healing and repair involve rebuilding tissues, restoring structure, and normalizing cell function. If immune signaling remains elevated, repair processes can’t complete properly. Some peptides directly support the body’s repair mechanisms by encouraging cell proliferation, enhancing collagen synthesis, or promoting extracellular matrix restoration. These activities support more complete healing, which in turn helps reduce the triggers that perpetuate inflammation.
Peptides Regulating Stress and Metabolic Pathways
Chronic inflammation often intertwines with metabolic stress — for example, when oxidative stress damages tissues, or when insulin resistance contributes to immune dysregulation. Certain peptides help support antioxidant pathways and metabolic balance, which reduces the cellular stress that fuels inflammatory signaling.
By addressing these underlying contributors, peptide therapies can offer a more comprehensive approach to inflammation — one that supports the body’s ability to heal rather than simply tamping down symptoms.
The Science Behind Peptide Applications
Peptide research is a rapidly evolving field, and scientists continually uncover new ways these molecules influence human biology. Some of the mechanisms identified in research include:
- Signaling immune cells to shift from a pro-inflammatory to a more balanced state
- Enhancing macrophage activity to promote efficient cleanup of damaged cells
- Supporting regulatory T-cells that help resolve inflammation once the threat has passed
- Encouraging fibroblast activity for tissue and extracellular matrix repair
- Modulating oxidative stress pathways that contribute to chronic tissue damage
Because peptides are naturally occurring or derived from structures found in the body, they tend to be well-tolerated when used appropriately. They work at the cellular communication level, which can make their effects both subtle and profound — gradually supporting balance and recovery over time.
Real-World Applications: Who Might Benefit?
Peptide support for inflammation isn’t reserved solely for people with diagnosed autoimmune diseases. It can be relevant for a range of conditions where chronic inflammation interferes with quality of life. This includes people living with:
- Persistent joint discomfort or low-grade arthritic pain
- Post-viral inflammatory symptoms
- Metabolic syndrome with associated inflammatory components
- Ongoing muscle or connective tissue inflammation from repetitive stress
- Subclinical inflammation linked to fatigue, brain fog, or mood changes
Some individuals pursue peptide therapy alongside lifestyle interventions — such as improved nutrition, restorative movement practices, and sleep optimization — to enhance recovery. Others work with clinicians to integrate peptides into broader strategies that include physical therapy, stress management, and targeted supplementation.
Importantly, peptide therapy is not a stand-alone “fix.” It is part of a multidisciplinary approach that considers the whole person — their health history, lifestyle, environment, and goals.
What to Expect From Peptide-Based Support
People engaging in peptide-based inflammation support often describe gradual improvements rather than immediate relief. This isn’t surprising, since the goal is to help the body recalibrate and heal at a biological level.
Commonly reported benefits include:
- Reduced sensation of stiffness and discomfort over time
- Improved tissue resilience and recovery after activity
- Greater balance in energy and mood
- Enhanced healing following injury or repeated strain
- Fewer flare-ups of chronic inflammatory symptoms
These outcomes emerge as part of a larger trajectory of recovery — one that prioritizes sustainable change rather than quick relief.
Safety, Monitoring, and Professional Guidance
Because peptides influence biological signaling, their use should be guided by a qualified clinician. Individual needs vary, and what works in one person’s case may not be appropriate in another. A healthcare provider can help determine which peptides are most relevant, assess any potential interactions with medications, and monitor results over time.
Proper dosing, sourcing, and follow-up are critical components of safe, effective peptide support. Unlike off-the-shelf supplements, medically guided peptide therapy is customized to each individual’s biology and symptom profile.
This level of oversight helps ensure that peptide support complements — rather than complicates — other aspects of health care.
Integrating Peptides Into a Broader Inflammation Strategy
Peptide therapy is most effective when integrated into a holistic approach to inflammation. This includes:
- Nutritional patterns that support balanced immune function
- Regular movement and strength work to support tissue health
- Sleep practices that help regulate immune cycles
- Stress-reduction techniques that minimize chronic immune activation
- Monitoring and addressing metabolic contributors like blood sugar balance
Peptides can be an important piece of this overall puzzle — helping the body communicate more effectively, recruit repair mechanisms, and reduce chronic inflammatory signaling when paired with these foundational practices.
Taking the Next Step With Knowledge and Support
If chronic inflammation has been part of your health story — whether for months or years — you’re not alone, and you’re not without options. For many people, understanding the biology beneath their symptoms is the first step toward meaningful improvement. From there, exploring targeted, science-based interventions like peptide therapy offers a path that’s grounded in healing rather than suppression.
For those curious to learn more about how peptides are specifically being used for inflammation reduction and healing, this resource offers a deeper dive into current clinical applications: peptides for inflammation — with detailed insights and links to reputable research and treatment strategies.
Final Thoughts: Inflammation Is a Process — Healing Is Too
Chronic inflammation doesn’t develop overnight, and it doesn’t resolve overnight either. It is the result of prolonged biological signaling that has lost its natural rhythm of activation and resolution. Addressing it requires patience, curiosity, and a willingness to explore strategies that support the body’s innate capacity to heal.
Peptides represent an exciting frontier in this journey — not because they are a miracle cure, but because they help realign communication pathways that have become dysregulated over time. When used thoughtfully and professionally, they can be an integral part of a recovery plan that is personalized, comprehensive, and rooted in a deeper understanding of human biology.
If you’re navigating chronic inflammation and looking for support that goes beyond temporary relief, exploring peptide-based strategies with a trusted clinician may offer fresh possibilities. The path to healing is rarely simple, but with the right tools and guidance, it can be deeply effective.