Abstract
Skin lesions that grow rapidly often generate clinical concern because they challenge the distinction between benign and malignant processes. Such lesions may exhibit swift cellular proliferation, local tissue distortion, and architectural changes that demand careful evaluation. Their unpredictable behavior, tendency to mimic aggressive neoplastic patterns, and potential to alter the surrounding skin integrity make them a significant subject of discussion in dermatology. Many of these growths follow characteristic phases, initially acceleration, a period of stabilization, and eventual transformation or resolution, yet recognizing these patterns requires experience and an understanding of cutaneous biology. Environmental influences, genetic predispositions, immune status, and external irritants frequently shape their development and progression. Because some lesions may resemble harmful conditions, clinicians often rely on timely assessment and appropriate therapeutic strategies to ensure both safety and optimal outcomes. In this article, we explore one such rapidly evolving cutaneous lesion known as keratoacanthoma and its management in the conventional medicinal system and in the traditional Indian medicinal system of Ayurveda.

Introduction
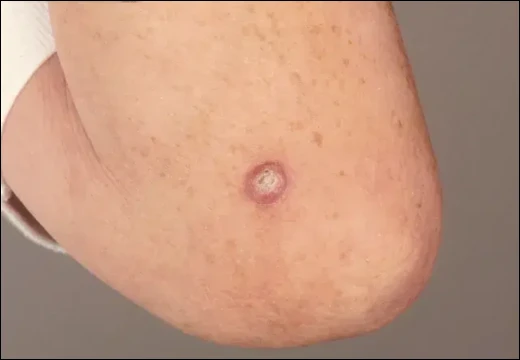
Keratoacanthoma (KA) is a distinctive epidermal tumor that originates from the pilosebaceous unit, typically displaying swift enlargement over a matter of weeks followed by a plateau phase and eventual spontaneous regression. Despite being historically classified as a benign lesion, it continues to occupy a controversial position in dermatopathology because of its close histological and behavioral similarity to well-differentiated squamous cell carcinoma (SCC). KA most often affects middle-aged to elderly individuals, especially those with fair skin frequently exposed to sunlight. The characteristic lesion appears as a dome-shaped nodule with a central keratin-filled crater, usually located on sun-exposed areas such as the face, neck, forearms, and hands. While solitary lesions are most common, some individuals experience multiple or eruptive forms due to genetic predispositions or underlying syndromes. Although many keratoacanthomas regress over months, clinical observation alone is risky because a lesion presumed to be KA may actually be SCC. Moreover, some KA lesions can behave aggressively, infiltrate local tissue, or fail to regress. Hence, understanding its etiology, clinical presentation, diagnostic approach, and management is crucial for safe and effective patient care.
Key Facts
- Keratoacanthoma is a rapidly growing cutaneous tumor arising from the hair follicle epithelium.
- Its clinical and histopathological appearance can closely mimic well-differentiated squamous cell carcinoma, making diagnosis challenging.
- Lesions typically develop rapidly within 2–6 weeks, stabilizing before slowly regressing over several months.
- Chronic exposure to ultraviolet (UV) radiation is the most significant environmental risk factor.
- It occurs most commonly on sun-exposed areas such as the face, forearms, neck, and hands.
- Most cases present as solitary nodules, although multiple or eruptive patterns may occur in certain genetic syndromes.
- Keratoacanthoma follows a triphasic growth pattern namely proliferation, maturation, and involution.
- Individuals over the age of 50, especially fair-skinned people, are at highest risk.
- Despite spontaneous regression in many cases, active treatment is preferred due to diagnostic overlap with SCC and potential for aggressive behavior.
Causes
1. Ultraviolet (UV) Radiation
Prolonged UV exposure, particularly UV-B radiation, is the leading environmental cause of KA. It induces:
- DNA damage in epidermal keratinocytes
- Reduced local immune surveillance
- Accelerated skin aging
- Mutations that lead to abnormal keratinocyte proliferation
People living in sunny climates or those with outdoor occupations are especially prone.
2. Genetic Factors
Genetics play a substantial role in certain forms of KA:
- Mutations in TGF-β signaling pathways (e.g., TGFBR1) are found in familial KA syndromes.
- Autosomal dominant conditions such as Ferguson-Smith syndrome and Grzybowski syndrome lead to multiple eruptive keratoacanthomas.
- Deficiencies in DNA repair (e.g., xeroderma pigmentosum) also predispose to tumor formation.
These genetic defects often cause dysregulated cell growth within the hair follicle unit.
3. Chemical Carcinogens
Exposure to irritants and carcinogenic substances can trigger KA in susceptible individuals:
- Tar and pitch
- Industrial oils
- Petroleum derivatives
- Herbicides and chemical irritants
These substances may cause keratinocyte mutations that set the stage for tumor development.
4. Immunosuppression
People with weakened immune systems have a notably higher risk of KA. This includes:
- Organ transplant recipients on long-term immunosuppression
- Individuals with HIV/AIDS
- Patients undergoing chemotherapy
- Those taking chronic corticosteroids
Impaired immunity reduces the body's ability to eliminate abnormal proliferating cells.
5. Viral Etiology (HPV)
Some studies have detected human papillomavirus (HPV) DNA in KA lesions. Although the causal role is not proven, certain HPV subtypes might act as co-factors in tumor development, especially in immunocompromised patients.
6. Trauma And The Koebner Phenomenon
KA can appear at the site of:
- Burns
- Surgical wounds
- Radiation scars
- Tattooed skin
- Chronic irritation
Trauma-induced inflammation may stimulate abnormal follicular keratinocyte growth.
7. Ionizing Radiation
Previous exposure to radiotherapy or environmental radiation can predispose to KA formation. Lesions may arise years after the radiation insult.
8. Tobacco Use
Smoking, especially pipe or cigar use, increases the risk of KA on the lips due to mucocutaneous exposure to carcinogens.
9. Advancing Age
Keratoacanthoma primarily affects individuals over 50 years due to:
- Cumulative sun damage
- Declining immune surveillance
- Increased genetic mutations with age
- Thinning of the epidermis and follicular changes
Thus, age itself is a significant risk factor.
Signs And Symptoms
Keratoacanthoma is characterized by a very distinctive clinical evolution, occurring in three stages: rapid proliferation, maturation, and eventual involution.
1. Proliferative Phase (Rapid Growth, 2–6 Weeks)
This is the hallmark feature of KA:
- Begins as a small erythematous or flesh-colored papule
- Rapidly expands into a dome-shaped nodule
- Growth is usually symmetric and can reach 1–2 cm quickly
- The surface is smooth, firm, and sometimes shiny
- Mild tenderness or a sensation of tightness may be reported
The rate of growth distinguishes KA from most other benign skin lesions.
2. Maturation Phase (Crater Formation)
During this period:
- The nodule develops a central keratin-filled crater
- Edges of the lesion become rolled or elevated
- The appearance becomes “volcano-like”
- Keratin material may accumulate, forming a thick plug
- The lesion is typically painless, although mild discomfort may persist
This phase is when KA most closely resembles squamous cell carcinoma.
3. Involution Phase (Spontaneous Regression, Months)
In this phase:
- Growth ceases, and the lesion begins to shrink
- The central plug may fall off
- The nodule gradually flattens
- Healing occurs with a scar, which may be atrophic or hyperpigmented
- The entire regression process may take several months
However, involution is not guaranteed, and some lesions persist or enlarge.
Additional Clinical Features
- Location: Most commonly occurs on the face (nose, cheeks, eyelids), neck, hands, and forearms.
- Texture: Firm and solid to palpation.
- Color: Flesh-colored, pink, or reddish.
- Size: Usually 1–3 cm but may grow larger (giant keratoacanthoma).
- Number: Typically solitary, but multiple types occur in genetic syndromes.
- Symptoms: Usually asymptomatic, though itching, mild pain, or bleeding may occasionally occur.
Features Suggestive Of Aggressive Behavior
- Continuous growth beyond normal size
- Ulceration with bleeding or crusting
- Invasion of surrounding tissues
- Persistent lesion without regression
- Recurrence after treatment
In such cases, prompt medical intervention is essential.
Investigations
- Dermoscopy
- Skin biopsy
- Histopathology
- CT scan
- MRI
- Lymph node ultrasound
Management
Since keratoacanthoma cannot be reliably distinguished from squamous cell carcinoma based on clinical examination alone, early active management is preferred over observation. Treatment depends on the lesion’s size, location, number, and patient characteristics.
- Surgical Excision
- Curettage and Electrodessication
- Intralesional Therapy
- Topical Therapies
- Systemic Therapy
- Cryotherapy
- Radiotherapy
Ayurvedic Aspect of Keratoacanthoma
Keratoacanthoma, though a modern dermatological diagnosis, can be correlated within Ayurveda through principles governing granthi (nodular swellings), vrana-shotha (inflammatory lesions), and pittaja or raktaja twak vikara (skin lesions involving Pitta dosha and Rakta dhatu). Ayurveda does not describe a single-condition equivalent to keratoacanthoma; however, its origin from the pilosebaceous unit, rapid proliferation, dome-shaped elevation, central keratinous plug, and eventual involution reflect a complex interplay of dosha imbalance, dhatu dushti, and agni distortions at the level of the skin (twak), blood (rakta), and muscle (mamsa).
Nidana And Samprapti (Causes And Pathophysiology)
In Ayurveda, the etiological factors contribute to dosha prakopa, primarily of Pitta and Rakta, followed by Kapha involvement leading to tissue overgrowth. Important nidanas include:
1. Excessive Exposure To Sunlight (Atapa Sevanam)
Keratoacanthoma is strongly linked to UV radiation. Ayurveda correlates excessive sun exposure with:
- Pitta prakopa (pitta dosha aggravation)
- Rakta dushti (blood vitiation)
- Twak dahata (burning and inflammation)
- Mandalotpatti (patches and nodules)
Modern photosensitive disorders align with “Bhrajaka (a subtype of pitta dosha) Pitta vitiation.”
2. Consumption Of Pitta-Alleviating Foods
Diets and habits that vitiate Pitta dosha and Rakta (blood) include:
- Spicy, sour, fermented foods
- Excess alcohol
- Salt-heavy diet
- Excessive oily or fried foods
These contribute to dermal inflammation.
3. Chronic Tobacco And Chemical Exposure
Ayurveda associates such irritants with:
- Raktadushti
- Mamsa dhatu vikriti
- Utklesha of Pitta-Kapha
4. Trauma-Induced Lesions (Abhighata)
Keratoacanthoma often arises from minor injury or post-surgical scars. In Ayurveda:
- Trauma can provoke Rakta and Mamsa vrana (wound/lesion)
- Leading to granthi-like (nodular) lesions
This relates to the “Sadyovrana → Dushta Vrana → Granthi” sequence.
5. Immunosuppression
Ayurveda correlates low immunity with:
- Ojas kshaya
- Vyadhikshamatva hani
- Rakta-vaha srotodushti
6. Genetic Predisposition
“Beeja dosha,” i.e., genetic distortions, leads to:
- Recurrent nodules
- Uncontrolled cellular proliferation in the follicles
All these causes lead to formation of Keratoacanthoma.
Signs And Symptoms In Ayurvedic Interpretation
- Vaivarnya (Discoloration)
- Styana or Ghana vriddhi (Firm Nodule)
- Madhyabhaga Shushkata (Central Dry Plug)
- Shotha (Localized Swelling)
- Alpa Vedana (Mild Pain)
- Druta Vriddhi (Rapid Growth)
Management In Ayurveda
Ayurvedic treatment strategy includes Shodhana (bio-purification), Shamana (palliative therapy), Rakta-shodhana (blood cleansing), Srotoshodhana (microchannel clearance), Rasayana (rejuvenation therapy), and local applications.
A. Shodhana Chikitsa (Bio-Purification)
1. Virechana (Purgation Therapy)
Indicated for:
- Pitta-Rakta dushti
- Inflammatory skin lesions
Virechana drugs such as Trivrit, Draksha, Aragwadh, Avipattikar choorna etc are used.
2. Raktamokshana (Bloodletting)
Leech therapy (Jalaukavacharana) is effective for raised, inflamed nodules.
B. Shamana Chikitsa (Pacifying Therapy)
1. Anti-Inflammatory And Pitta-Pacifying Herbs
Anti-inflammatory and Pitta-Pacifying Herbs are used such as Neem (Azadirachta indica), Manjistha (Rubia cordifolia), Sariva (Hemidesmus indicus), Guduchi (Tinospora cordifolia)
2. Kapha-Pacifying Herbs
Kapha-Pacifying Herbs for Granthi and Swelling such as Kanchnar (Bauhinia variegata), Varuna (Crataeva nurvala), Turmeric (Curcuma longa).
3. Vata-Anulomana
To regulate rapid uncontrolled growth such as Castor oil microdoses, Trivrut avaleha, Eranda-based formulations.
C. External Applications
1. Herbal Pastes (Lepa)
- Manjistha + Haridra + Neem paste can be applied over the lesion as it acts as anti-inflammatory and aids regression of the same.
- Panchavalkala Kashaya Lepa is astringent and reduces the size of the lesion.
2. Taila And Ghrita Applications
- Jatyadi Taila helps in deep healing and softens the keratin plug.
- Kumkumadi Taila prevents hyperpigmentation.
D. Rasayana Therapy
Rasayanas promote normal tissue regeneration after lesion regression.
- Amla Rasayana helps to enhance collagen and immunity.
- Chyawanprash promotes balanced digestion and healthy skin.
- Guduchi Rasayana rebuilds immunity and restores cellular integrity.
E. Diet And Lifestyle
Avoid
- Excess sun exposure
- Spicy, acidic foods
- Smoking
- Alcohol
- Chemical cosmetics
Include
- Cooling foods
- Bitter vegetables
- Herbal teas
- Proper sleep
- Skin protection
Herbal Remedies For Keratoacanthoma By Planet Ayurveda
Planet Ayurveda is a globally trusted Ayurvedic brand known for delivering pure, authentic, and highly effective herbal formulations. Built on the principles of classical Ayurveda, the company focuses on promoting natural healing through time-tested herbs, traditional preparation methods, and strict quality standards. Every product at Planet Ayurveda is crafted with carefully selected medicinal plants sourced from clean and sustainable environments, ensuring maximum potency and safety. The brand emphasizes a holistic approach to wellness, offering solutions that address the root cause of health challenges rather than just symptoms. From immunity and digestion to skin, joints, liver health, and chronic conditions, Planet Ayurveda provides a wide range of herbal supplements and classical formulations prepared with precision. Their commitment to purity—free from chemicals, preservatives, and artificial ingredients—makes them a preferred choice for people seeking natural, side-effect-free alternatives. With a growing global presence, Planet Ayurveda continues to spread the ancient wisdom of Ayurveda in a modern, reliable, and accessible way. Planet Ayurveda is pleased to present its list of products that are quite beneficial in the management of Keratoacanthoma.
Herbal Remedies For Keratoacanthoma
Product List
- Kanchnaar Guggul
- Kaishore Guggul
- Crab Go Capsule
- Chandraprabha Vati
- Telomere Boostup
- Crab Curcumin 95%
Product Description
1. Kanchnaar Guggul
Kanchnaar Guggul is a well-known classical ayurvedic formulation used in the management of various swellings, tumors, and cystic growths. The key herb, Kanchnaar (Bauhinia variegata), along with Guggul (Commiphora mukul) and others work nicely to reduce abnormal tissue proliferation and inflammation. The formulation helps manage the condition primarily through its anti-inflammatory and anti-tumor properties. Kanchnaar acts as a potent detoxifier and lymphatic cleanser, promoting the breakdown of pathological growths and reducing Kapha dosha and Rakta (blood) vitiation associated with skin swellings. Guggul enhances this effect by providing anti-inflammatory actions that reduce swelling and redness, while also exhibiting cytotoxic properties that help regulate abnormal cell proliferation and support the resolution of tumours. Additionally, Kanchnaar Guggul improves metabolic activity and supports detoxification, which enhances tissue healing and prevents recurrence. This combined action makes Kanchnaar Guggul a valuable support in the management aimed at shrinking the lesion, preventing further growth, reducing inflammation, and promoting tissue repair in keratoacanthoma.
Dosage: Two tablets twice a day.
2. Kaishore Guggul
Kaishore Guggul is a classical ayurvedic medicine composed of Guggulu (Commiphora mukul), Amla (Emblica officinalis), Haritaki (Terminalis chebula), Vibhitaki (Terminalia bellerica), Guduchi (Tinospora cordifolia), Sonth (Zingiber officinalis), Maricha (Piper nigrum), Pippali (Piper longum), Vidanga (Embelia ribes), Red Physic Nut, and Indian Jalap, helps in the management of Keratoacanthoma through a blend of anti-inflammatory, detoxifying, and antioxidant actions. Its active chemical constituents such as guggulsterones, ellagic acid, gallic acid, chebulinic acid, berberine, flavonoids, tannins, and lignans play a crucial role in reducing oxidative stress and regulating abnormal keratinocyte activity. These compounds help suppress inflammatory mediators and enhance tissue repair and immune response. The formulation’s strong Rakta-shodhana (blood cleansing) effect aids in clearing metabolic toxins and maintaining healthy skin physiology. Its antioxidant rich herbs neutralize free radicals that contribute to dysregulated cell turnover, whereas its digestive and metabolic regulators help reduce endotoxins preventing further tissue aggravation. Together, these phytochemicals and classical herbs create a multi-dimensional protective effect that supports natural healing and stabilizes the lesion, making Kaishore Guggul a beneficial adjunct in the management of keratoacanthoma.
Dosage: Two tablets twice a day.
3. Crab Go Capsule
Crab Go Capsules are a product of Planet Ayurveda and contains a blend of herbs such as Ashwagandha (Withania somnifera), Shatavari (Asparagus racemosus), Turmeric (Curcuma longa), Tulsi (Ocimum sanctam), and other supportive herbs, collectively offering anti-inflammatory, antioxidant, cytotoxic, and immunomodulatory benefits. The active phytochemicals present in the herbs such as withanolides, curcuminoids, saponins, and flavonoids help regulate abnormal cellular signaling and suppress excessive tissue growth. Compounds like withaferin A show strong anti-proliferative and pro-apoptotic activity, encouraging abnormal cells to undergo natural regression. Turmeric’s curcuminoids assist in reducing oxidative stress and inflammatory cytokines, thereby limiting the triggers that drive rapid lesion expansion. Additionally, the formulation boosts immune response, helping the body recognize and respond appropriately to atypical skin cells. Its detoxifying and rejuvenating actions maintain healthier Rakta (blood) and Mamsa dhatus (muscle tissue). Altogether, Crab Go Capsule offers supportive internal protection that aids in stabilizing and managing keratoacanthoma.
Dosage: Two capsules twice a day.
4. Chandraprabha Vati
Chandraprabha Vati is a classical Ayurvedic formulation comprising a blend of a number of potent herbs and minerals known for their anti-inflammatory, detoxifying, and rejuvenating properties. In this condition, it helps by balancing aggravated doshas, particularly Pitta and Kapha. Its anti-inflammatory properties help reduce swelling and redness associated with the lesion. The formulation contains herbs like Shilajit (Asphaltum), Guduchi (Tinospora cordifolia), Amla (Emblica officinalis), Haritaki (Terminalis chebula) and Vibhitaki(Terminalia bellerica) and other ingredients which work collectively to detoxify the body by eliminating toxins (ama) and improving metabolic function. This detoxification and immune modulation aid in controlling abnormal cell proliferation and promote healing. Moreover, Chandraprabha Vati enhances tissue regeneration and maintains mucosal and skin health by its antioxidant and tissue-nourishing actions. It supports the body's immune response to prevent secondary infections and chronic inflammation. Overall, Chandraprabha Vati acts as a systemic immunomodulator and detoxifier, contributing to reducing lesion size, controlling inflammation, and promoting repair and preventing recurrence of Keratoacanthoma.
Dosage: Two tablets twice a day.
5. Telomere Boostup
Telomere Boostup is a product of Planet Ayurveda that contains potent herbs such as Giloy (Tinospora cordifolia), Ashwagandha (Withania somnifera), Grape Seed extract (Vitis vinifera), Amla (Emblica officinalis) etc which provide a strong therapeutic basis for managing keratoacanthoma through their active constituents and pharmacological effects. Giloy (Tinospora cordifolia) is rich in alkaloids like berberine, which exhibit significant anti-inflammatory and immunomodulatory properties, helping reduce inflammation and enhance immune response around skin lesions. Ashwagandha (Withania somnifera) contains withanolides known for antioxidant, anti-inflammatory, and anti-proliferative effects, which help regulate abnormal cell growth and support tissue repair. Grape Seed (Vitis vinifera) extract is high in proanthocyanidins and polyphenols that offer powerful antioxidant and anti-cancer activities; these compounds protect skin cells from oxidative damage, inhibit tumor cell proliferation, and induce apoptosis in abnormal cells. Amla (Emblica officinalis) contributes with its vitamin C and polyphenols, enhancing antioxidant defense, promoting collagen synthesis, and stimulating skin healing. Together, these bioactive constituents act synergistically by reducing oxidative stress, modulating immune function, downregulating inflammatory pathways, and promoting cellular repair and regeneration. This multi-faceted mechanism supports the reduction of lesion progression, prevention of secondary infection, and restoration of healthy skin architecture, making Telomere Boostup an effective addition to the management plan of Keratoacanthoma.
Dosage: One capsule twice a day.
6. Crab Curcumin 95%
Crab Curcumin 95% is a potent herbal supplement formulated by Planet Ayurveda that contains a concentrated extract of curcumin, the principal bioactive compound found in turmeric (Curcuma longa) and marich (Piper nigrum). Its powerful anti-inflammatory, antioxidant, and anti-proliferative properties make it highly beneficial in managing keratoacanthoma. Curcumin directly impacts the inflammatory pathways involved in the condition by downregulating pro-inflammatory cytokines such as TNF-α, IL-6, and NF-kB, thereby reducing swelling and redness around the lesion. Its antioxidant capacity neutralizes free radicals and oxidative stress. Furthermore, curcumin has demonstrated anti-cancer effects by inducing apoptosis (programmed cell death) in abnormal cells and inhibiting pathways related to cancer cell survival and metastasis. Its immunomodulatory effects strengthen the body's defense system to prevent secondary infections and support healing of keratoacanthoma lesions. The high bioavailability formula ensures better absorption and efficacy, making it an effective add on in Ayurvedic management to control lesion progression, inflammation, and promote overall skin health.
Dosage: One capsule twice a day.
Conclusion
Keratoacanthoma is a unique dermatological condition that demands a careful, multidisciplinary approach because of its rapid growth and resemblance to squamous cell carcinoma. While many lesions may regress spontaneously, clinical observation alone is often unsafe, making timely diagnosis and active management essential. Understanding its multifactorial origin including ultraviolet exposure, genetic susceptibility, immunosuppression, chemical irritants, and trauma, allows for better preventive and therapeutic planning. Ayurveda provides an additional holistic framework that explains the condition through the lens of Pitta-Kapha imbalance, Rakta dushti, and srotas obstruction, offering supportive strategies through detoxification, blood purification, anti-inflammatory herbs, and rejuvenation therapies. Integrating modern dermatological treatment with Ayurveda’s systemic and local interventions enhances the overall outcome, promotes healthy tissue regeneration, and prevents recurrence. The products mentioned in the text are helpful in supporting skin health, balancing aggravated doshas, improving immunity, and aiding natural tissue repair that gets damaged from Keratoacanthoma. With a thoughtful combination of modern medical care, Ayurvedic wisdom, lifestyle modifications, and targeted herbal support, patients can achieve better control over the condition and maintain long-term skin wellness.