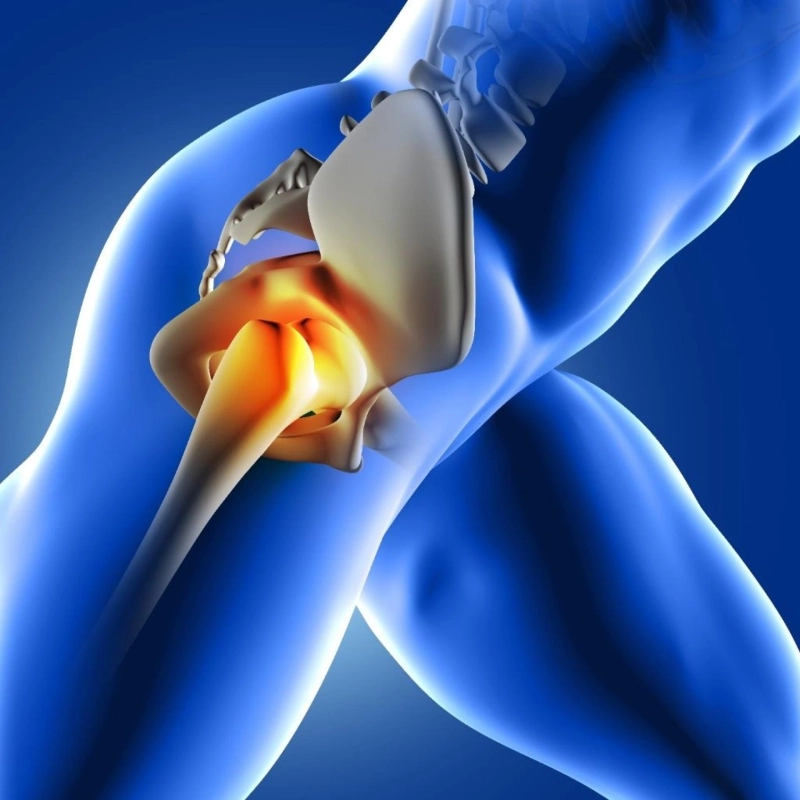
The hip is a ball-and-socket joint where the top of your thigh bone (femur) fits into the pelvic socket. When this joint’s cushioning cartilage wears away or the bones are badly damaged, it can cause severe pain and stiffness. Hip replacement surgery (also called total hip arthroplasty) is a procedure where an orthopaedic surgeon removes the damaged parts of the hip joint and replaces them with metal and plastic components. These artificial parts (a prosthetic ball and socket) mimic the hip’s normal movement. In most cases, hip replacement dramatically reduces pain and restores function. The goal of this surgery is to improve quality of life by relieving pain and improving mobility after the joint has been worn out or injured.
The hip joint connects your leg to your pelvis and works like a classic “ball and socket.” (The ball is the femur head, and the socket is part of the pelvic bone.) During hip replacement surgery, a surgeon removes the diseased bone and cartilage and inserts artificial components. This new joint acts like a cushion, helping reduce pain and improve motion.
Hip replacements are most often done when arthritis or injury has severely damaged the hip joint. For example, osteoarthritis (wear-and-tear arthritis) is the most common cause: over time, the cartilage in the hip joint wears down, eventually causing “bone-on-bone” grinding that leads to intense pain and stiffness. Other causes include inflammatory arthritis (like rheumatoid arthritis) or loss of bone from poor blood flow (osteonecrosis). In general, doctors only recommend hip replacement when other treatments have failed, and the pain is bad enough to seriously affect daily life. Mayo Clinic notes that hip replacement might be considered if your hip pain “interferes with daily activities” and nonsurgical treatments no longer help.
Common Symptoms and Signs
How do you know your hip problem is serious enough to consider surgery? The key warning signs are symptoms that your hip joint is badly damaged. Specialists look for things like:
- Persistent, severe hip or groin pain: The hip pain is constant or comes back repeatedly, and it limits everyday activities or even rest.
- Reduced mobility or stiffness: You have trouble bending, walking, or moving. Simple tasks like putting on shoes, climbing stairs, or getting out of a chair become painful or nearly impossible.
- Pain at rest or at night: Hip pain that doesn’t go away when you rest, that wakes you from sleep, or that even hurts when you’re sitting still is a red flag.
- No relief from treatments: You have tried medicines, anti-inflammatory drugs, physical therapy, injections or other therapies, but the pain persists.
- Changes in walking: You limp or can’t walk normal distances. You may need a cane or walker to get around comfortably.
- Grinding, clicking, or swelling: You might feel or hear a grinding, popping or “creaking” in the hip, and the joint may be tender, red or swollen due to inflammation.
- Impact on life and mood: Hip pain has started affecting your sleep, work, hobbies or mental health. If chronic pain makes you irritable, depressed or keeps you from activities you enjoy, that signals your quality of life is suffering.
- Doctor’s findings: Sometimes other causes (back or knee problems) must be ruled out first. If your doctor has checked for these and concludes the hip itself is the problem, then hip replacement might be needed.
If you notice one or more of these warning signs, talk to your doctor about the cause. Orthopaedic surgeons will perform a thorough exam and likely order imaging (like an X-ray) to see how badly the hip joint is worn or damaged. They may test your range of motion and strength to confirm the diagnosis. As one source puts it, if your hip pain has “reduced your mobility and this prevents you from working or sleeping, and other treatments have failed, it may be time to consider surgery.
Why It Might Be Time
In short, hip replacement surgery is usually considered only after conservative treatments haven’t given enough relief. For many people, that means trying medications (like pain relievers and anti-inflammatories), weight loss, exercise or physical therapy first. If those measures “no longer work, then surgery becomes the likely option. Mayo Clinic gives this rule of thumb: replacement may be an option if hip pain is severe enough to affect your daily routines (walking, climbing stairs, even sleeping) and nonsurgical treatments have failed.
For example, if you find you need to take pain pills every day just to get by, or if you can’t bend your hip without sharp pain, these are signals that the hip joint may be worn out. Similarly, feeling a “catch” or grinding deep in the hip during movement can indicate cartilage is gone. These problems often stem from arthritis reaching an advanced stage. In osteoarthritis, especially, all the cushioning cartilage can wear away, as one NIH image description notes, “virtually all of the cartilage around the top of the femur bone deteriorates, leading to grinding and pain.
In practice, the decision often comes down to quality of life. If your hip pain is making you avoid walking, causes you to sleep poorly, or keeps you from work or hobbies, then hip replacement can give you back your ability to enjoy life. After careful examination and imaging, your surgeon can advise whether a new hip prosthesis is warranted.
Recovery and Outlook
Hip replacement is a major surgery, and recovery takes time. After surgery, you will likely spend a short time in the hospital, then go home with crutches or a walker. Physical therapy is an important part of recovery: you will be guided through exercises to regain strength and range of motion in your new hip. Mayo Clinic notes that many patients are “doing well” by about three months after surgery, and they continue to improve over the first year. With a successful replacement, most people experience much less pain and a much better ability to move than before. The new hip helps you walk further and stand more easily. However, it’s generally advised to avoid very high-impact activities (like running or jumping) on the new joint. In time, most patients can resume low-impact sports such as swimming, cycling or golfing with their new hip.
It’s worth knowing that hip implants are durable but not permanent. Many artificial hips last 15–20 years or more. Younger or more active patients may eventually need a “revision” surgery if the implant wears out earlier. But modern implant materials have greatly improved longevity. The most important thing is how much the surgery improves your life now. For example, one report notes that a replaced hip “can reduce pain and increase the hip’s range of motion, helping people get back to enjoying everyday activities.
Overall, hip replacement is a common and generally successful surgery. Millions of patients have found relief from chronic hip pain and restored mobility through this procedure. If your hip pain is one of the key signs listed above, it may be time to discuss hip replacement with an orthopaedic specialist.
Summary
Hip replacement surgery is a well-established treatment for severe hip pain caused by advanced arthritis or injury. You may need it when you have persistent hip pain, stiffness, or loss of motion that makes daily activities difficult and isn’t helped by other treatments. Key signs include chronic pain, difficulty walking, pain at night, or hip grinding/noise. If you see an orthopaedic doctor with these symptoms, they will evaluate your hip (including range-of-motion tests and X-rays) to decide if replacement is the right step. Recovery takes time, but most patients find that a new hip relieves pain and restores mobility, allowing them to return to a more active life.