 Introduction
Introduction
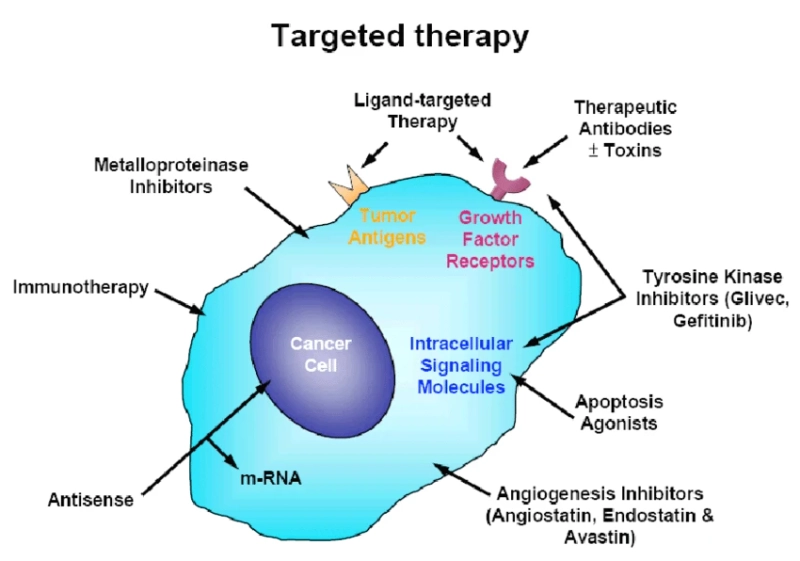
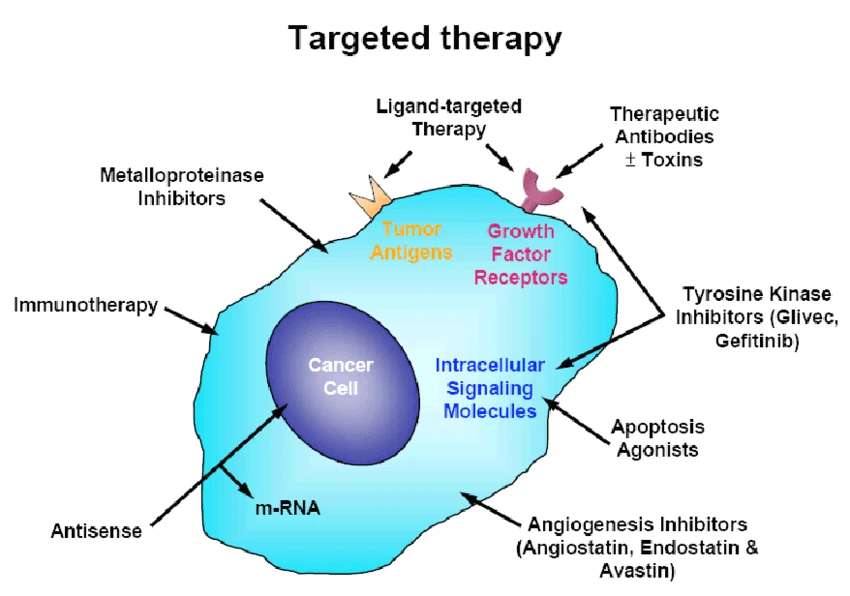
Targeted therapy represents a major advancement in cancer treatment, offering a more precise, focused approach compared to traditional chemotherapy. Unlike chemotherapy — which affects both cancerous and healthy fast-dividing cells — targeted therapy works by interfering with specific molecules involved in cancer cell growth, progression, and survival. This treatment option is particularly valuable in haemato-oncology, where it has shown success in conditions like chronic myeloid leukemia (CML), certain types of lymphoma, and multiple myeloma.
What is Targeted Therapy?
Targeted therapy refers to drugs or substances that block the growth and spread of cancer by interfering with specific molecules (often proteins) that cancer cells rely on. These molecules may be involved in cell signaling, growth factor receptors, or mutated genes driving cancer progression.
This form of treatment is also known as molecular targeted therapy or precision therapy, and it falls under the broader category of personalized medicine — where therapy is selected based on the individual genetic profile of a patient’s cancer.
How Does Targeted Therapy Work?
Targeted therapies work in various ways to inhibit cancer growth:
- Blocking signals that tell cancer cells to grow or divide.
- Interrupting blood supply to tumors by targeting vascular endothelial growth factor (VEGF).
- Inducing apoptosis (programmed cell death).
- Delivering toxins directly into cancer cells through antibody-drug conjugates.
- Targeting specific gene mutations or proteins such as BCR-ABL, HER2, or EGFR.
Unlike chemotherapy, targeted therapies aim to spare most normal, healthy cells, thereby reducing many of the systemic side effects.
Common Types of Targeted Therapy
1. Monoclonal Antibodies
These are laboratory-made proteins that bind to specific antigens on cancer cells. Some act as flags for the immune system, while others block important cancer cell functions.
Examples:
- Rituximab (targets CD20 in B-cell lymphomas)
- Trastuzumab (targets HER2 in breast cancer)
- Daratumumab (targets CD38 in multiple myeloma)
2. Tyrosine Kinase Inhibitors (TKIs)
These are small-molecule drugs that block enzymes called tyrosine kinases involved in cell signaling.
Examples:
- Imatinib (used in CML, targets BCR-ABL)
- Dasatinib, Nilotinib (next-generation TKIs)
- Ibrutinib (targets BTK in certain lymphomas)
3. Proteasome Inhibitors
These block the action of proteasomes, which cancer cells use to dispose of damaged proteins.
Examples:
- Bortezomib
- Carfilzomib (used in multiple myeloma)
4. Angiogenesis Inhibitors
These block the formation of new blood vessels that tumors need to grow.
Example:
- Bevacizumab (anti-VEGF therapy)
Targeted Therapy in Haemato-Oncology
Targeted therapy has revolutionized the treatment of blood cancers. Here are key examples:
1. Chronic Myeloid Leukemia (CML)
- Imatinib was the first targeted therapy introduced, drastically improving survival.
- CML is characterized by the BCR-ABL gene fusion, which can be selectively targeted.
2. Non-Hodgkin’s Lymphoma
- Rituximab, an anti-CD20 monoclonal antibody, is now standard in B-cell lymphomas.
3. Multiple Myeloma
- Targeted monoclonal antibodies like Daratumumab and Elotuzumab are now integral to treatment plans.
- Proteasome inhibitors are also key players in therapy regimens.
4. Chronic Lymphocytic Leukemia (CLL)
- Ibrutinib (BTK inhibitor) and Venetoclax (BCL-2 inhibitor) have transformed the therapeutic landscape.
How is Targeted Therapy Administered?
Targeted therapy can be administered in different ways:
- Oral tablets or capsules (e.g., TKIs like Imatinib)
- Intravenous (IV) infusion (e.g., Rituximab, Daratumumab)
- Some treatments require hospital visits, while others can be taken at home.
Treatment may be used alone or in combination with chemotherapy, immunotherapy, or stem cell transplantation, depending on the type and stage of cancer.
Advantages of Targeted Therapy
- 🎯 Precision: Acts only on cancer cells with specific targets.
- 💊 Fewer side effects compared to traditional chemotherapy.
- ⏱️ Prolonged disease control in certain blood cancers.
- 🧬 Option for personalized treatment based on genetic mutations.
- 🔄 Synergy with other therapies to improve outcomes.
Limitations and Challenges
- Cancer cells can develop resistance over time.
- Not all cancers have known or actionable targets.
- Molecular testing is required before treatment, which may not always be accessible or affordable.
- Some side effects, while fewer, can still be serious.
Common Side Effects of Targeted Therapy
Although generally better tolerated than chemotherapy, targeted therapies can cause:
- Skin rashes
- Fatigue
- Diarrhea
- Liver enzyme elevation
- High blood pressure (especially with angiogenesis inhibitors)
- Risk of infections (in monoclonal antibody therapy)
- Blood clotting issues (in some therapies)
Patients on targeted therapy require regular monitoring through blood tests and clinical evaluation.
Role of Genetic Testing
Before initiating targeted therapy, doctors may recommend molecular or genetic testing (also known as biomarker testing). These tests help identify mutations or proteins that can be targeted effectively. For example:
- BCR-ABL in CML
- CD20 in lymphoma
- BRAF, EGFR, or ALK in solid tumors
Such testing ensures that the patient receives a therapy that is most likely to work for their unique cancer type.
Duration of Treatment
Targeted therapy is often taken continuously for months or even years, especially in chronic conditions like CML or CLL. The duration depends on:
- Response to treatment
- Tolerance to side effects
- Disease progression or relapse
Some patients achieve deep, durable remissions and may eventually stop therapy under supervision.
Targeted Therapy vs. Chemotherapy
FeatureChemotherapyTargeted TherapyActionKills all fast-dividing cellsAttacks specific cancer moleculesSide EffectsMore widespreadOften milderPersonalizationNot based on geneticsGenetically tailoredDeliveryMostly IVOral or IVPrecisionLowHigh
Targeted Therapy and the Future of Cancer Care
As research advances, more cancers are being linked to specific mutations, leading to the discovery of new targeted agents. The rise of next-generation sequencing (NGS) and companion diagnostics is accelerating this progress.
Future directions include:
- Combination of targeted therapy with immunotherapy
- Development of next-gen inhibitors for resistant cancers
- Bispecific antibodies and cell-based therapies with targeted mechanisms
Conclusion
Targeted therapy marks a significant step forward in oncology, especially in haemato-oncology where it has revolutionized treatment for several blood cancers. By focusing on the specific biology of each patient’s disease, targeted therapies offer improved survival rates, better quality of life, and fewer side effects. As science evolves, targeted therapy is expected to become an integral part of most cancer treatment strategies.