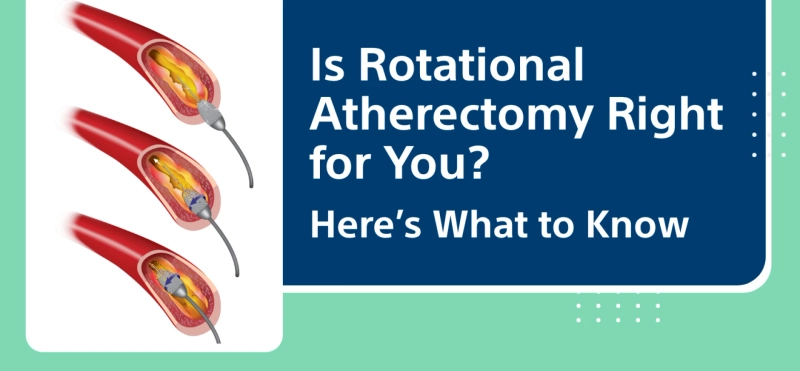
Rotational atherectomy represents a specialized form of interventional cardiology designed to tackle stubborn, calcified plaques that obstruct coronary arteries. When standard balloon angioplasty cannot adequately dilate a hardened lesion, patients and clinicians may ponder whether rotational atherectomy treatment offers the necessary solution. This high-speed, diamond-coated burr spins to “sand away” calcified plaque, thereby facilitating stent delivery and expansion. As with any advanced procedure, one must weigh the benefits against rotational atherectomy risks.
What is Rotational Atherectomy?
Rotational atherectomy represents a specialised form of interventional cardiology designed to address stubborn, calcified plaques that impede coronary arteries. When trendy balloon angioplasty can't competently dilate a hardened lesion, sufferers and clinicians may additionally contemplate whether or not rotational atherectomy therapy offers the vital solution.
This high-pace, diamond-coated burr spins to “sand away” calcified plaque, thereby facilitating stent shipping and enlargement. As with any advanced procedure, one must weigh the advantages in opposition to rotational atherectomy risks.
Understanding Calcified Coronary Disease
Coronary arteries, once in a while, develop calcified plaques—hardened, calcium-wealthy deposits which can resist traditional interventional strategies. Unlike softer, lipid-weighted down plaques that balloon angioplasty easily compresses, calcified lesions continue to be inflexible and regularly recoil, preventing full vessel expansion. Patients with excessive calcification may also experience persistent angina no matter of previous stent placement or medicinal drug optimization.
On angiography, these plaques appear as radiopaque, white regions within the vessel wall, signaling an improved challenge. Heavily calcified segments additionally growth the danger of incomplete stent apposition, leading to higher rates of restenosis or stent thrombosis. Recognizing calcified coronary ailment early—based on imaging or failure of a balloon to completely open—units the stage for thinking about rotational atherectomy as a means of creating a smoother lumen and improving procedural success.
The Procedure Step by Step
Before any rotational atherectomy dangers are borne, a radical assessment unfolds. Coronary angiography first quantifies the degree and place of calcification. Renal feature, coagulation profile, and medicine records (inclusive of antiplatelet sellers) are reviewed. On the day of the process, the patient arrives at the catheterization lab under aware sedation or, once in a while, general anesthesia—depending on complexity.
Vascular get admission to is established through a radial or femoral artery sheath. A guiding catheter advances the specialized guidewire across the goal lesion. The diamond-lined burr is then threaded over the twine. Using a controlled “pecking” approach—brief, cautious advances and retreats—the operator sands away calcium, taking care to hold burr runs underneath 30 seconds to restrict warmness era and decrease the chance of gradual-float phenomena.
Fluoroscopic steering guarantees particular positioning, mainly around bends or ostial plaques. Once sufficient debulking takes place, low-strain balloon angioplasty follows, creating an area for correct stent deployment. Finally, a drug-eluting stent generally tacks the newly widened lumen open. Total cath lab time can range from 60 to 120 minutes, with most rotational atherectomy intervals lasting just a few minutes.
Weighing Benefits: Why Choose Rotational Atherectomy?
Rotational atherectomy remedy offers several key benefits while handling inflexible, calcified coronary disease.
• First, it significantly improves stent expansion and apposition. Without ok lesion instruction, stents can underexpand—a predictor of restenosis and stent thrombosis. By sanding away the calcium, the burr creates an extra compliant vessel wall, permitting drug-eluting stents to fully deploy.
• Second, success charges in complex, calcified lesions rise dramatically. Studies have shown that procedural success in heavily calcified segments exceeds 90 percent, whilst rotational atherectomy precedes balloon angioplasty versus far lower fees with balloon angioplasty alone.
• Third, rotational atherectomy can make previously untreatable segments—consisting of an ostial right coronary lesion—amenable to stenting. For many sufferers, this indicates avoiding more invasive surgical treatment.
• Finally, long-term patency improves for the reason that fully extended stents reduce neointimal hyperplasia. When comparing options like cutting balloons, rotational atherectomy regularly gives you more predictable and durable outcomes in extreme calcification.
Understanding the Risks and Limitations
As with any intervention, rotational atherectomy includes inherent rotational atherectomy dangers. Microembolization is possibly the most commonplace: microscopic particles of calcium can dislodge and migrate downstream, causing slow-flow or no-reflow phenomena that manifest as chest ache, hypotension, or maybe brief myocardial dysfunction.
Vessel perforation or dissection, even as rare, can arise if the operator overadvances the burr or applies excessive force, mainly in skinny or tortuous vessels. Transient coronary heart block may additionally broaden whilst the burr passes through the proximal right coronary artery, necessitating transient pacing in pick instances.
Arrhythmias can also occur through excessive-speed burr activation, requiring vigilant ECG monitoring. Beyond those device-specific dangers, preferred PCI dangers remain: vascular get entry to headaches (hematoma, pseudoaneurysm), evaluation-brought on nephropathy, and allergies to contrast dye.
Some lesions still defy even the maximum experienced operators—for instance, very long, diffuse calcifications or segments with excessive tortuosity. In those instances, operators would possibly abandon rotational atherectomy because of safety worries, opting instead for alternative strategies.
Also Read: Navigating Atrial Fibrillation: Tips for a Balanced Heartbeat
Recovery, Follow-Up, and Long-Term Outlook
After finishing rotational atherectomy and stent placement, patients generally spend several hours in a monitored recuperation vicinity, then are admitted to a telemetry or step-down unit. Radial get admission to frequently allows ambulation within a few hours; femoral access may additionally necessitate bed rest for 4–6 hours to reduce bleeding risk. Dual antiplatelet therapy (aspirin plus a P2Y12 inhibitor) is critical, typically for at least one year if a drug-eluting stent has been placed. Statin therapy is intensified to stabilize plaques elsewhere, at the same time as blood pressure and diabetes control get hold of close interest.
Cardiac rehabilitation, with supervised exercise and dietary counseling, aids in risk discount and purposeful restoration. Follow-up visits typically consist of symptom evaluation and, if indicated, non-invasive strain testing or CT angiography.
Patients must remain vigilant for chest soreness, signs and symptoms of access-site complications (bruising, swelling), or signs and symptoms suggestive of restenosis. Long-time period effects hinge on both the most excellent lesion guidance via rotational atherectomy and diligent scientific and lifestyle adherence—smoking cessation, weight loss plan change, and regular physical activity.
Conclusion and Key Takeaways
When coronary arteries harbor extreme calcification that defeats conventional balloon angioplasty, rotational atherectomy regularly fills the distance—transforming rigid, untreatable plaques into a extra compliant channel for stenting.
As a precision “sanding” device, the diamond-tipped burr improves stent apposition, reduces procedural failure rates, and complements lengthy-time period vessel patency. Yet, rotational atherectomy risks—which include microembolization, vessel perforation, or arrhythmias—necessitate cautious patient selection and operator information.
Alternatives like scoring balloons, reducing balloons, or intravascular lithotripsy can also apply in much less extreme instances or whilst burr-primarily based therapy includes undue risk. Ultimately, candidacy hinges on lesion anatomy, comorbidities, and a radical heart-crew discussion.
For sufferers suffering with “undilatable” calcified blockages, rotational atherectomy treatment can offer renewed hope—provided they understand both its robust blessings and its potential complications. If heavy calcium burdens your coronary arteries, discussing rotational atherectomy with your interventional cardiologist may pave the way to better blood flow and improved quality of life.