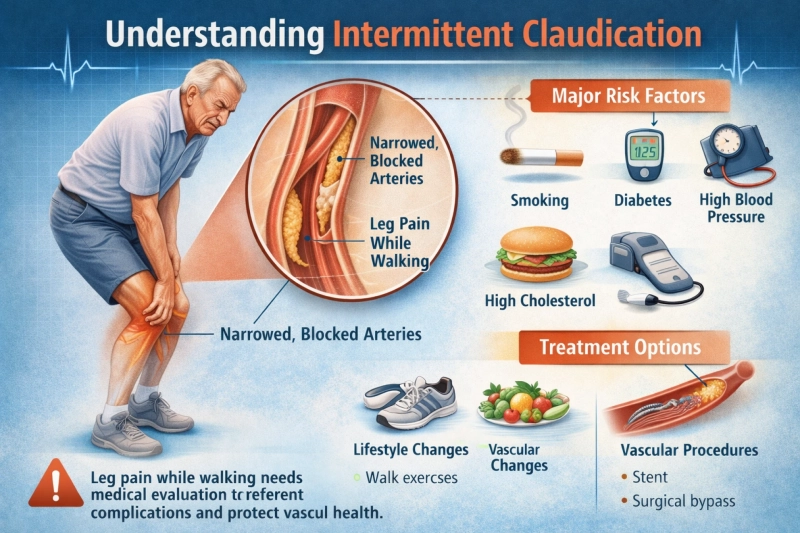
Intermittent claudication is a common symptom of peripheral artery disease (PAD) that affects blood flow to the legs. It usually presents as leg pain while walking that improves with rest. Although often ignored in early stages, intermittent claudication can be an important warning sign of underlying vascular disease.
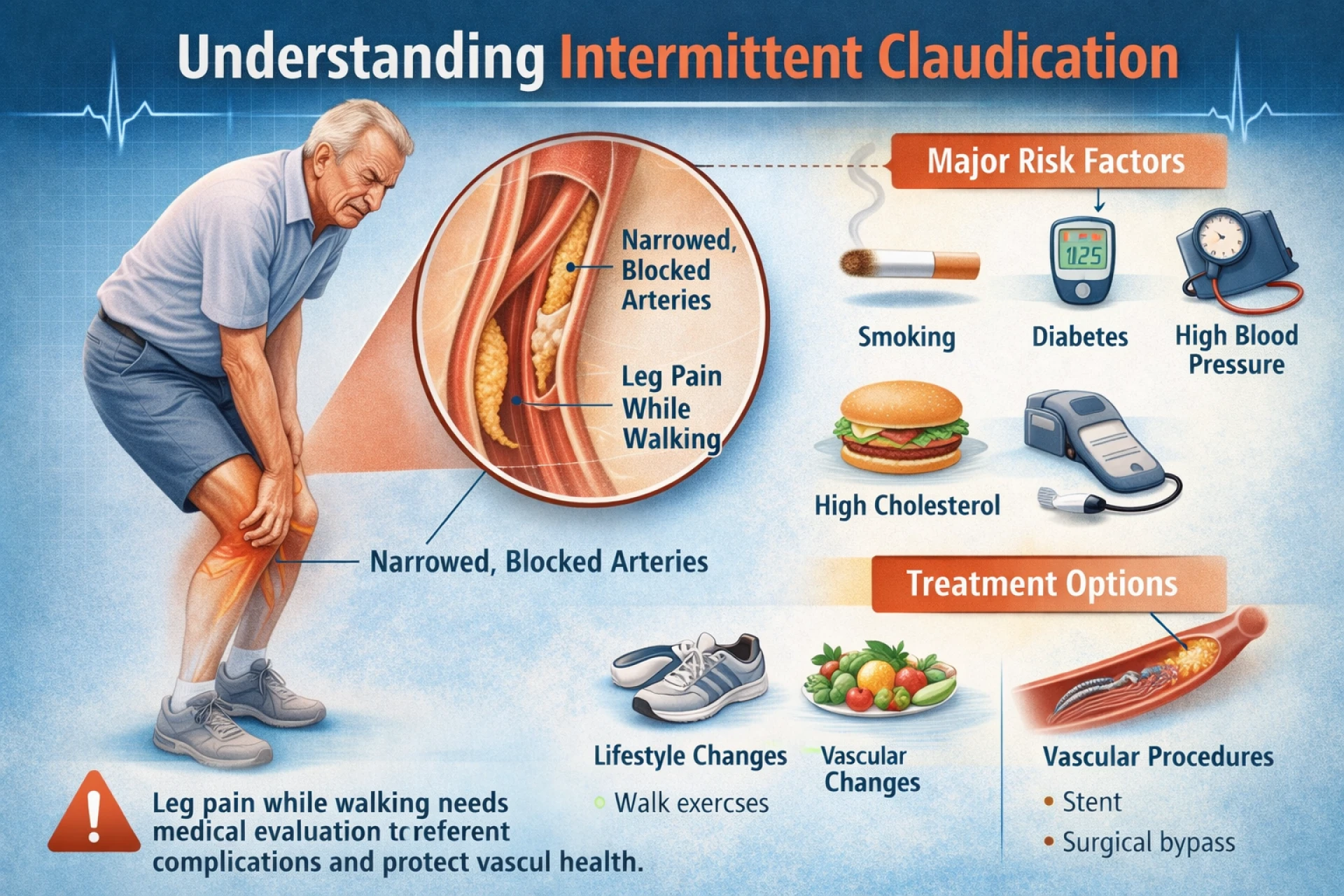
What Is Intermittent Claudication?
Intermittent claudication refers to muscle pain or cramping in the legs caused by reduced blood supply during physical activity. The pain typically occurs in the calves but may also affect the thighs, hips, or buttocks. Once the person stops walking and rests, the pain usually subsides within a few minutes.
Why Does Intermittent Claudication Occur?
The most common cause of intermittent claudication is narrowing or blockage of leg arteries due to atherosclerosis. When muscles need more oxygen during walking, restricted blood flow cannot meet the demand, leading to pain.
Common causes include:
- Peripheral artery disease (PAD)
- Fatty plaque buildup in arteries
- Reduced oxygen supply to leg muscles
- Long-standing vascular narrowing
Common Symptoms to Watch For
Symptoms may vary from mild discomfort to severe pain. Early recognition is important to prevent progression.
Typical symptoms include:
- Cramping or aching pain in calves during walking
- Leg heaviness or fatigue
- Pain relieved by rest
- Coldness in lower legs or feet
- Weak or absent foot pulses
- Slow-healing foot wounds (in advanced cases)
Risk Factors for Intermittent Claudication
Certain conditions increase the risk of developing intermittent claudication and peripheral arterial disease.
Major risk factors:
- Smoking
- Diabetes
- High blood pressure
- High cholesterol
- Obesity
- Increasing age
- Sedentary lifestyle
People with heart disease or stroke history are also at higher risk.
How Is Intermittent Claudication Diagnosed?
Diagnosis usually involves a combination of clinical examination and vascular tests.
Common diagnostic methods include:
- Ankle-Brachial Index (ABI) test
- Doppler ultrasound of leg arteries
- CT or MR angiography (if required)
- Physical examination of leg pulses
Early diagnosis helps guide appropriate treatment and lifestyle changes.
Treatment Options for Intermittent Claudication
Treatment focuses on improving blood flow, reducing symptoms, and preventing disease progression.
Non-surgical management:
- Supervised walking exercise programs
- Smoking cessation
- Blood pressure and cholesterol control
- Blood-thinning medications
- Diabetes management
Advanced treatment options (when needed):
- Angioplasty and stenting
- Minimally invasive vascular procedures
- Surgical bypass in severe cases
The choice of treatment depends on symptom severity and arterial blockage.
Lifestyle Changes That Can Help
Lifestyle modification plays a crucial role in managing intermittent claudication.
Helpful changes include:
- Regular walking exercises
- Healthy, balanced diet
- Weight management
- Avoiding tobacco use
- Proper foot care
These steps not only improve symptoms but also reduce cardiovascular risk.
When Should You Seek Medical Advice?
You should consult a vascular specialist if:
- Leg pain limits daily activities
- Pain worsens over time
- Wounds on legs or feet do not heal
- You experience rest pain or numbness
Ignoring symptoms may lead to critical limb ischemia, a serious condition requiring urgent care.
Conclusion
Intermittent claudication is more than just leg pain—it is often a sign of underlying vascular disease. Early diagnosis, lifestyle changes, and appropriate treatment can significantly improve mobility and quality of life. Understanding symptoms and seeking timely medical evaluation are key steps toward protecting long-term vascular health.